| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Carotid Artery Dissection
Related Subjects: |Neurological History taking |Causes of Stroke |Ischaemic Stroke |Subarachnoid Haemorrhage |Cerebral Arterial Perfusion and Clinical Correlates |Anterior circulation Brain |Posterior circulation Brain |Acute Stroke Assessment (ROSIER&NIHSS) |Carotid Artery dissection |Vertebral artery dissection |Acute Stroke Assessment (ROSIER&NIHSS) |Atrial Fibrillation |Atrial Myxoma |Causes of Stroke |Ischaemic Stroke |Cancer and Stroke |Cerebral Venous thrombosis |Cardioembolic stroke |CT Basics for Stroke |Endocarditis and Stroke |Haemorrhagic Stroke |Stroke Thrombolysis |Hyperacute Stroke Care |AP of the Brain |Cryptogenic stroke |Carotid Web |Anterior / Medial Medullary Infarct (Dejerine Syndrome)
🧠 Introduction
- Carotid dissection (CD) accounts for only 1–2% of all ischaemic strokes, but in young and middle-aged adults it causes up to 10–25% of strokes.
- Posterior circulation dissections (vertebral) are also important but less common than carotid.
- Key teaching: Carotid/vertebral dissection without suspicion of SAH is not a contraindication to thrombolysis.
- Always ask about unusual neck trauma (e.g. chiropractor, sports injury, yoga, sneezing) in a young patient with stroke.
⚙️ Aetiology & Pathophysiology
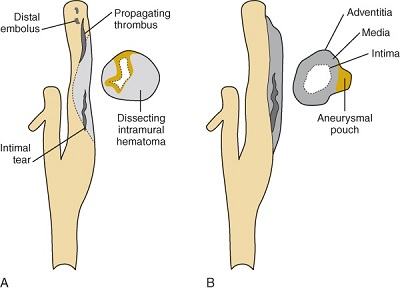
- Dissection = tear in the intimal layer → blood enters vessel wall → intramural haematoma.
- Source of blood: through intimal tear (luminal blood) or rupture of vasa vasorum (or both).
- Consequences:
- 🩸 Luminal narrowing or occlusion.
- 🧩 Endothelial damage → thrombosis → artery-to-artery embolisation.
- ⚠️ Rarely, extension intracranially → subarachnoid haemorrhage (SAH).
- Rationale for therapy = prevent thrombus/embolisation and maintain flow.
📊 Epidemiology
- Always suspect in young adults (<50) with anterior circulation stroke.
- Prognosis is generally good with low recurrence risk.
- Carotid dissections ≈3× more common than vertebral dissections.
- Typical site: internal carotid artery, 2–3 cm distal to bifurcation.
- Genetic/structural predispositions: Marfan’s, Ehlers–Danlos IV, fibromuscular dysplasia (only ~2%).
- Males = females in prevalence; peak incidence = mid-40s.
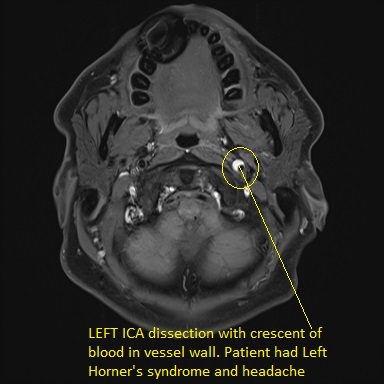
🩺 Clinical Features
- 🧠 TIA/stroke (most common).
- 🪖 Neck, face, or retro-orbital pain.
- 👁️ Ipsilateral Horner’s syndrome (ptosis, miosis, enophthalmos – but usually no anhidrosis).
- 🧩 Migrainous-type headache.
- 👅 Hypoglossal nerve palsy (due to compression).
- 🫀 PACI/TACI-type stroke due to carotid occlusion or MCA emboli.
- ⚡ Rare: SAH if dissection extends intracranially → thunderclap headache.
💡 Classic triad: unilateral neck pain + Horner’s syndrome + ischaemic stroke = think carotid dissection.
⚡ Common Triggers & Associations
- Violent sneeze, cough, or vomiting.
- Sports: cricket, rugby, rowing, football.
- Neck extension/rotation: yoga, painting ceilings, hairdresser basin.
- Minor trauma: road traffic accidents, blow to head.
- Chiropractic manipulation (may be causal or just association).
- Recent respiratory infection, migraine, or resuscitation procedures.




🔍 Imaging
- 📸 CTA or MRA: Best non-invasive tests; ultrasound often misses dissections above jaw angle or vertebral arteries.
- 🧲 MRI T1 fat-suppression: shows crescentic wall haematoma = classic crescent sign.
- 📉 Angiography (DSA/CTA/MRA): tapered stenosis, “string sign”, or occlusion.
- 🧠 MRI DWI: detects embolic infarcts in affected territory.
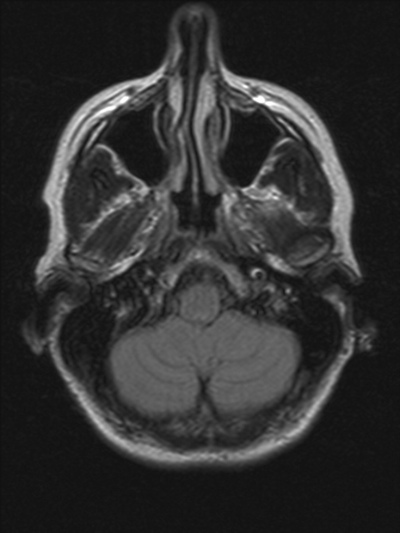
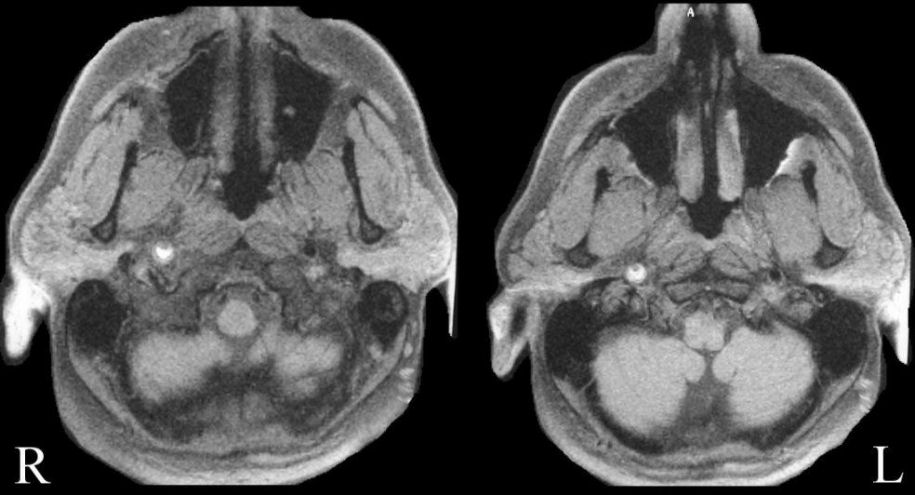
⚖️ Management
- 🩹 ABC + acute stroke therapies: IV thrombolysis or thrombectomy are appropriate. Dissection alone is not a contraindication.
- 💊 Antithrombotic therapy:
- Antiplatelets (aspirin, clopidogrel) often preferred in practice.
- Anticoagulation (warfarin/DOAC) reasonable alternative; CADISS trial showed no difference between strategies.
- 📅 Duration: typically 3–6 months, then reassess with repeat imaging.
- ⚠️ Intracranial dissections: higher SAH risk → anticoagulation less favoured.
- 📉 Recurrence risk is low; avoiding provoking mechanism is key.
💡 Exam Pearl: Young adult with stroke + neck trauma + Horner’s → think carotid dissection. Antithrombotics reduce early risk; no proven benefit of anticoagulation over antiplatelets.
📚 Further Reading
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
