| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Acute Abdomen - Perforation of a Viscus
Related Subjects:Acute Cholecystitis |Acute Appendicitis |Chronic Peritonitis |Acute Abdomen - Perforation of a Viscus |Abdominal Aortic Aneurysm |Ectopic Pregnancy |Acute Cholangitis |Acute Abdominal Pain |Penetrating Abdominal Trauma |Abdominal Masses: Clinical Approach and Considerations |Abdominal Distension |Vomiting
🩻 CT scan abdomen is the gold standard and more sensitive than plain films for suspected GI perforation. ⚠️ Findings may be masked in elderly or immunosuppressed patients.
📖 About
- Perforation of a gas- and bacteria-containing GI tract anywhere from oesophagus ➝ anus.
- 💨 Gas rises and can be seen trapped under the diaphragm on an erect CXR.
- Perforation leads to free intraperitoneal air and spillage of luminal contents → bacterial peritonitis + sepsis.
🧬 Aetiology
- Can occur at any point in the GI tract.
- Always consider in any patient presenting with an acute abdomen.
- Free air = red flag for overwhelming bacterial peritonitis and septic shock if untreated.
📸 Imaging: Free Air
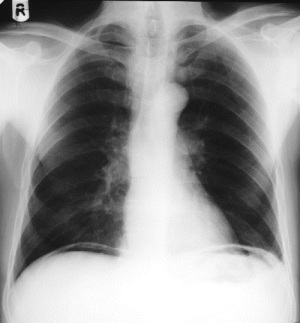
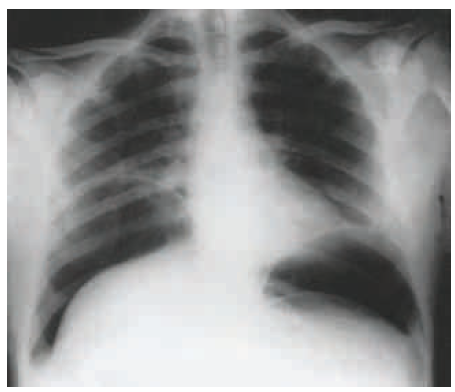
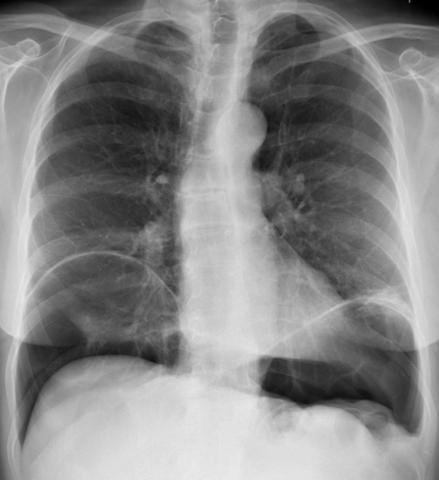
⚠️ Causes
- Oesophagus: Caustic ingestion, endoscopic biopsy/dilatation, Boerhaave syndrome (post-vomiting), oesophageal tumour, chest trauma.
- Stomach: Peptic ulcer disease, NSAID-induced erosion, gastric cancer, penetrating trauma.
- Small bowel: Ischaemia, Crohn’s disease (fistula/erosion), trauma.
- Large bowel: Toxic megacolon (C. difficile, UC), diverticulitis, polypectomy/perforation during colonoscopy, trauma, cancer.
🩺 Clinical Features
Findings may be subtle in elderly or chronically immunosuppressed patients.
- 🚨 Sudden severe abdominal pain, worsened by movement.
- Rigidity, rebound, and percussion tenderness (“board-like abdomen”).
- Absent bowel sounds.
- Fever, tachycardia, hypotension (sepsis/shock).
- May coexist with bowel obstruction, diverticulitis, or malignancy.
🔍 Differentials
- Acute pancreatitis
- Myocardial infarction (can mimic upper abdo pain)
- Tubo-ovarian pathology (ruptured cyst, torsion)
- Ruptured abdominal aortic aneurysm (AAA)
🧪 Investigations
- 🩸 Bloods: FBC, U&E, LFTs, amylase, CRP – often raised WCC/CRP.
- 🩻 Plain films: CXR/AXR → free air under diaphragm, Rigler’s sign (air both sides of bowel wall), loss of psoas outline.
- 💧 Contrast swallow → useful if oesophageal perforation suspected.
- 🖥️ CT Abdomen = gold standard (sensitive for free air, perforation site, complications).
💉 Management
- 🚫 Nil by mouth (NPO).
- ABC resuscitation: IV fluids, oxygen, monitoring, analgesia.
- Broad-spectrum IV antibiotics (cover Gram-negatives + anaerobes).
- Immediate surgical review:
- Perforation repair or resection (laparotomy/laparoscopy).
- Selected cases (contained leak, stable patient) → conservative management with close observation.
- Consider ITU/HDU support if unstable.
📚 References
- NICE guidance on acute abdomen and GI emergencies.
- BNF – Antibiotic regimens for intra-abdominal sepsis.
- RCS guidelines on management of hollow viscus perforation.
📝 Revisions
- Updated September 2025
3 Clinical Cases - Gastrointestinal Perforation of a Viscus ⚠️🩻
- Case 1 - Perforated peptic ulcer 🥼: A 48-year-old man with a history of NSAID use presents with sudden-onset severe epigastric pain radiating to the shoulder. He lies motionless, abdomen rigid with rebound tenderness. CXR: free air under the diaphragm. Teaching: A perforated duodenal ulcer is the classic cause of acute peritonitis with “board-like” abdomen. Urgent surgical repair (e.g. Graham patch) + IV fluids, antibiotics, and NG tube decompression are indicated.
- Case 2 - Perforated diverticulitis 🌿: A 72-year-old woman with left lower quadrant pain, fever, and constipation develops worsening peritonitis and hypotension. CT abdomen: sigmoid diverticulitis with free air and fluid. Teaching: Diverticular perforation often presents in older patients and carries high mortality. Management depends on severity: IV antibiotics, percutaneous drainage if contained abscess, or emergency colectomy with stoma (Hartmann’s procedure) for free perforation.
- Case 3 - Iatrogenic perforation (colonoscopy) 💉: A 64-year-old man undergoes colonoscopy for polyp surveillance and develops acute abdominal pain and tachycardia post-procedure. AXR: large amount of free intraperitoneal air. Teaching: Colonoscopic perforation is a recognised complication. Prompt recognition is vital - management ranges from conservative (if stable, small perforation, minimal peritonitis) to urgent surgical repair. Always suspect when abdominal pain occurs after endoscopy.
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
