| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Pemphigoid Gestationis (Herpes Gestationis) ✅
Related Subjects: |Nikolsky's sign |Koebner phenomenon |Erythema Multiforme |Pyoderma gangrenosum |Erythema Nodosum |Dermatitis Herpetiformis |Lichen Planus |Acanthosis Nigricans |Acne Rosacea |Acne Vulgaris |Alopecia |Vitiligo |Urticaria |Basal Cell Carcinoma |Malignant Melanoma |Squamous Cell Carcinoma |Mycosis Fungoides (Sezary Syndrome) |Xeroderma pigmentosum |Bullous Pemphigoid |Pemphigus Vulgaris |Seborrheic Dermatitis |Pityriasis/Tinea versicolor infections |Pityriasis rosea |Scabies |Dermatomyositis |Toxic Epidermal Necrolysis |Stevens-Johnson Syndrome |Atopic Eczema/Atopic Dermatitis |Psoriasis
🤰 About Pemphigoid Gestationis (Herpes Gestationis)
- Pemphigoid Gestationis is a rare autoimmune blistering disorder of pregnancy. The historical name Herpes Gestationis is misleading because the condition is not caused by the herpes virus.
- The older term arose because early vesicles resembled herpes lesions, but histology and immunology confirm it is an autoimmune bullous dermatosis.
- Incidence: approximately 1 in 20,000–50,000 pregnancies.
- Most cases begin during the second or third trimester, although onset in late pregnancy or immediately postpartum can occur.
- The disease results from maternal autoantibodies directed against basement membrane proteins, particularly BP180 (type XVII collagen).
🧾 Clinical Features
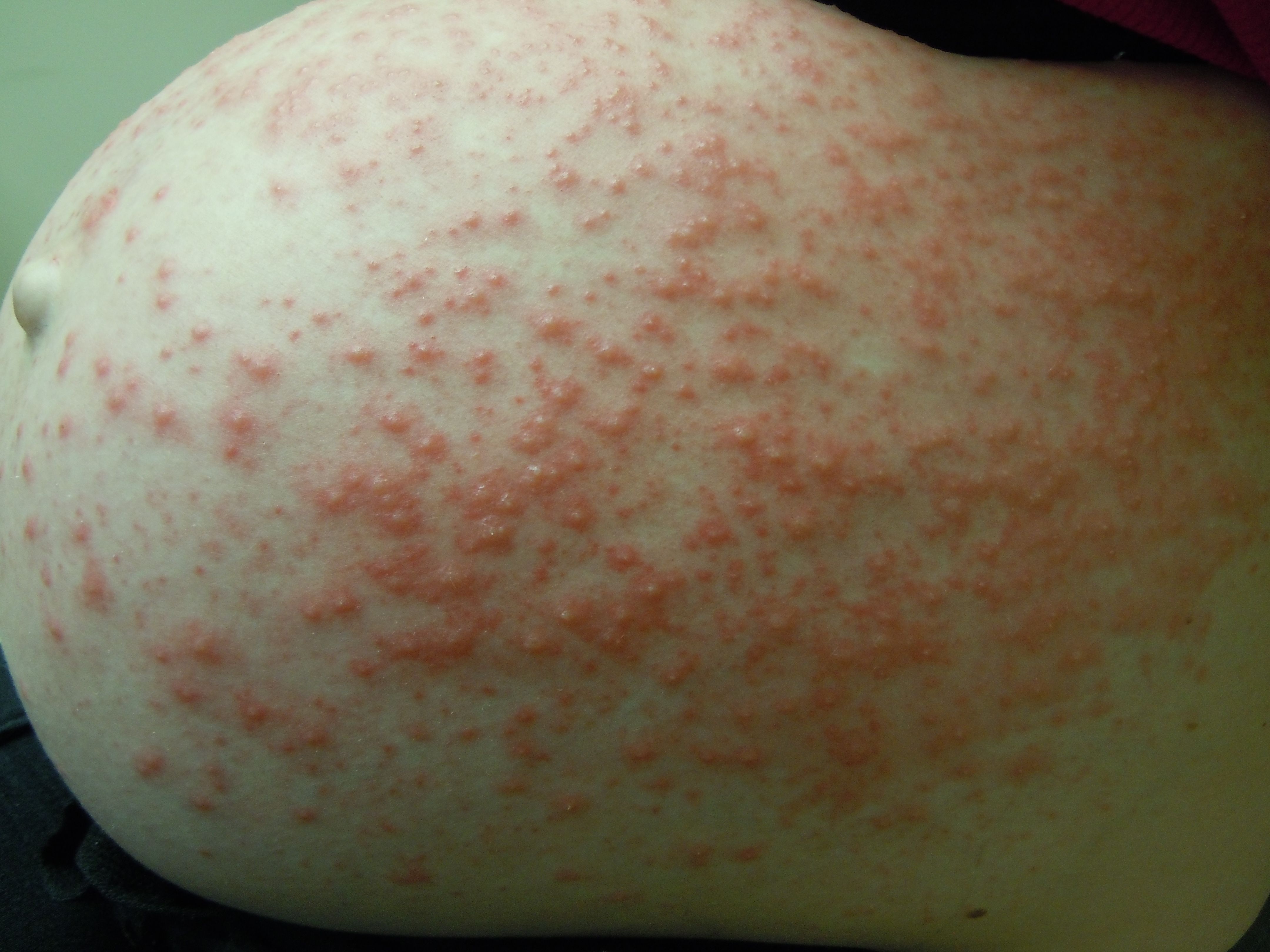
- Usually begins with intense pruritus, followed by urticarial plaques and papules.
- These lesions progress to vesicles and tense bullae.
- The rash classically begins around the umbilicus and then spreads to the trunk and limbs.
- Face and mucous membranes are usually spared.
- Pathophysiology: maternal IgG autoantibodies target hemidesmosomal proteins (especially BP180), activating complement and causing subepidermal blistering.
- Direct Immunofluorescence: Linear deposition of C3 (± IgG) along the basement membrane zone.
- Neonatal involvement: Rare; transient blisters may occur due to transplacental maternal IgG.
- A postpartum flare is common before gradual resolution.
- The condition frequently recurs in future pregnancies, often earlier and more severely.
🔬 Investigations
- Skin Biopsy: Taken from the edge of an active blister, showing subepidermal blistering with eosinophil-rich inflammatory infiltrate.
- Direct Immunofluorescence (DIF): Linear deposition of C3 (± IgG) at the basement membrane zone – the key diagnostic test.
- Indirect Immunofluorescence: May detect circulating antibodies against basement membrane proteins.
- ELISA testing: Can identify antibodies to BP180 (NC16A domain) and sometimes BP230.
- Blood tests: Usually normal; mild eosinophilia may occasionally be present.
💊 Management
- Mild disease: Emollients and potent topical corticosteroids are first-line to control inflammation and itching.
- Symptom relief: Oral antihistamines may help reduce pruritus.
- Moderate to severe disease: Oral prednisolone is usually required, with the dose tailored to disease severity.
- Specialist care: Management typically involves joint dermatology and obstetric review.
- Pregnancy monitoring: Obstetric follow-up is recommended due to a small increased risk of preterm delivery and low birth weight.
- Postpartum course: Symptoms usually resolve after delivery, although flares can occur shortly after birth.
- Future risk: Recurrence is common in subsequent pregnancies and may also occur with combined oral contraceptive use.
📚 Guideline & Evidence Sources
- Guidance on autoimmune blistering diseases from the British Association of Dermatologists (BAD).
- Dermatology and pregnancy reviews in the Royal College of Obstetricians and Gynaecologists clinical literature.
- UK prescribing and safety information from the British National Formulary (BNF).
- Clinical overview resources such as DermNet NZ, widely used in dermatology education.
- General pregnancy care recommendations from the National Institute for Health and Care Excellence (NICE).

Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
