| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Calcium Pyrophosphate Deposition (Pseudogout)
Related Subjects: |Calcium Physiology |Rheumatoid arthritis |Systemic Sclerosis (Scleroderma) |RA vs OA |Acute and Chronic Gout |Calcium Pyrophosphate Deposition (Pseudogout)
💡 Always aspirate the joint if diagnosis is uncertain to rule out septic arthritis 🔴. Send fluid for: cell count + Gram stain (Microbiology), polarizing microscopy for crystals (Histopathology), and culture. Record colour, viscosity, and turbidity of aspirate.
🦴 About
- Pseudogout = calcium pyrophosphate dihydrate (CPPD) crystal deposition disease.
- Described in 1962 by Kohn et al. Common in older adults, but can appear earlier if metabolic associations present.
- Favours large joints: knees, wrists, hips, pubic symphysis.
⚡ Aetiology
- Excess inorganic pyrophosphate → CPPD crystals deposit in articular & periarticular tissues.
- Age-related cartilage degeneration, genetic predisposition, or secondary to metabolic disease.
🔗 Associations
- Haemochromatosis
- Hypothyroidism
- Hyperparathyroidism
- Hypomagnesaemia
- Wilson’s disease
- Bartter syndrome
- Amyloidosis, Ochronosis
- Haemophilia
📸 Imaging: Chondrocalcinosis
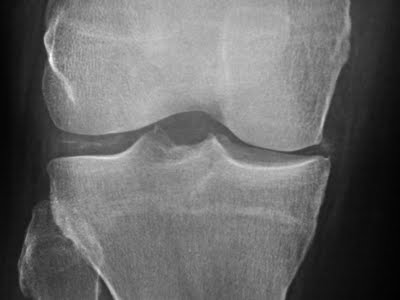
🔥 Clinical Features
- Acutely inflamed, hot, red, swollen, tender joint.
- Typically monoarticular (large joints), but can be oligo/polyarticular.
- Subacute or prolonged attacks (weeks–months).
- More common in elderly; in young patients think metabolic causes (e.g. haemochromatosis, Wilson’s).
🧪 Investigations
- Bloods: FBC, ESR/CRP ↑, U&E, calcium (for hyperparathyroidism), ferritin (haemochromatosis).
- Blood cultures: if septic arthritis in differential.
- X-ray: Linear calcification of hyaline or fibrocartilage = chondrocalcinosis.
- Joint aspirate: Rhomboid crystals, positively birefringent 🔬.
📊 Gout vs Pseudogout
| Feature | Gout | Pseudogout (CPPD) |
|---|---|---|
| Crystal | Monosodium urate | Calcium pyrophosphate |
| Shape | Needle-shaped | Rhomboid |
| Birefringence | Negative (yellow with parallel light) | Positive (blue with parallel light) |
| Typical Joint | 1st MTP (big toe) | Knee, wrist, hip |
| Peak Symptoms | Hours | Days (slower onset, longer course) |
💊 Management
- Acute attack:
- Rule out septic arthritis (aspirate first!).
- NSAIDs 🔵 (if tolerated, +PPI).
- Colchicine 0.5 mg BD for several days.
- Prednisolone 10–15 mg PO short course if NSAIDs/colchicine unsuitable.
- Admit if septic arthritis suspected.
- Chronic / recurrent disease:
- Hydroxychloroquine or Methotrexate in persistent inflammatory arthritis.
- Prophylaxis: low-dose colchicine or NSAID (with PPI).
- No urate-lowering equivalent: Unlike gout, no crystal-reducing therapy exists for CPPD.
