| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Conjunctivitis
👁️ Conjunctivitis (inflammation of the conjunctiva) is one of the most common causes of red eye. ⏳ Most cases are benign and self-limiting (7–10 days), but persistence, pain, or visual loss warrant urgent referral. 🦠 Infective conjunctivitis is usually viral and does not routinely require antibiotics. ⚠️ Always ask about contact lens use - risk of Pseudomonas keratitis.
📖 About
- The conjunctiva = thin mucous membrane lining the eyelids + sclera.
- Highly vascular → easily inflamed, causing redness, discharge, irritation.
- Spread via fingers, towels, or respiratory droplets → good hygiene essential.
🧾 Aetiology
- 🦠 Viral: Adenovirus (most common), enterovirus, HSV.
- 🧫 Bacterial: Strep pneumoniae, Staph aureus, H. influenzae, Moraxella. Hyperacute = gonococcal (sight-threatening!).
- 🤧 Allergic: Hay fever, atopy, seasonal allergens. Drug-induced (e.g., chloramphenicol).
- 🌍 Chronic: Trachoma (Chlamydia trachomatis) → scarring, blindness in endemic regions.
- ⚠️ Other: Autoimmune (Stevens–Johnson, cicatricial pemphigoid).
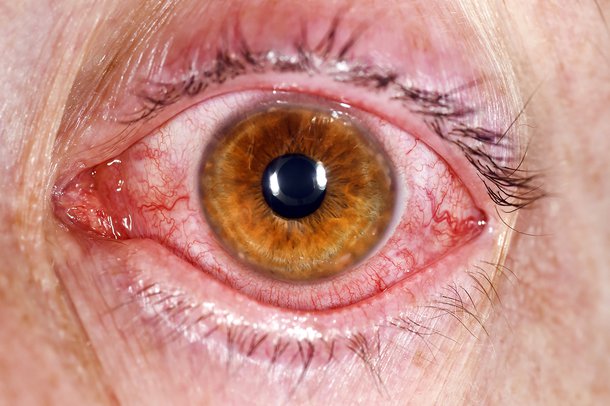
🔎 Clinical Features
- ⏱️ Resolves spontaneously in 7–10 days (if simple infective).
- 👁️ Red/pink eye with gritty sensation.
- Bacterial: Mucopurulent discharge, “glued” eyelids on waking.
- Viral: Watery discharge, often following URTI; highly contagious.
- Allergic: Bilateral, intense itching, stringy discharge, seasonal recurrence.
- STI-related: Gonococcal → copious purulent discharge, rapid corneal ulceration. Chlamydial → chronic, follicles, preauricular lymphadenopathy.
🧪 Investigations
- Usually clinical diagnosis.
- Swabs/culture if: atypical, recurrent, severe, or non-resolving.
- NAATs if chlamydia/gonorrhoea suspected.
- Slit-lamp exam if keratitis, uveitis, or foreign body suspected.
💊 Management
- General Measures (all types): 🧼 Hand hygiene, avoid sharing towels, no contact lenses until resolved.
- Allergic conjunctivitis: ❄️ Cool compresses, lubricants, topical antihistamines (olopatadine, azelastine). Mast cell stabilisers (sodium cromoglicate) for recurrent cases.
- Infective conjunctivitis: 💧 Lubricants for comfort. Most adults = viral → no antibiotics. Children with mucopurulent discharge may receive chloramphenicol if severe.
- Bacterial (purulent): Chloramphenicol 0.5% drops q2h × 48h → then QDS until 48h after resolution. Alternative: Fusidic acid gel BD (esp. children or compliance issues).
- STI-related: 🚨 Ophthalmia neonatorum (gonococcal) → emergency admission. IV/IM ceftriaxone + topical therapy. Chlamydial → systemic azithromycin/doxycycline + sexual health referral.
🚩 Red Flags - Refer Ophthalmology Urgently
- 👓 Contact lens wearers (risk of pseudomonal keratitis).
- 🩸 Pain, photophobia, or ↓ vision (uveitis, keratitis).
- ⚠️ Copious purulent discharge (gonococcal).
- 🧪 Suspected STI-related conjunctivitis.
- Recurrent or persistent >10 days despite treatment.
📚 References
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
