| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Squamous Cell Carcinoma
Related Subjects: |Nikolsky's sign |Koebner phenomenon |Erythema Multiforme |Pyoderma gangrenosum |Erythema Nodosum |Dermatitis Herpetiformis |Lichen Planus |Acanthosis Nigricans |Acne Rosacea |Acne Vulgaris |Alopecia |Vitiligo |Urticaria |Basal Cell Carcinoma |Malignant Melanoma |Squamous Cell Carcinoma |Mycosis Fungoides (Sezary Syndrome) |Xeroderma pigmentosum |Bullous Pemphigoid |Pemphigus Vulgaris |Seborrheic Dermatitis |Pityriasis/Tinea versicolor infections |Pityriasis rosea |Scabies |Dermatomyositis |Toxic Epidermal Necrolysis |Stevens-Johnson Syndrome |Atopic Eczema/Atopic Dermatitis |Psoriasis
📖 About
- Squamous Cell Carcinoma (SCC) is a malignant tumour of keratinocytes arising from the epidermis.
- It is the second most common skin cancer after basal cell carcinoma (BCC).
- SCC is locally invasive and slower growing than melanoma, but unlike BCC it carries a real risk of metastasis.
- Most often found on sun-exposed skin in older adults.
🌞 Causes / Risk Factors
- UV radiation (sunlight or tanning beds) - cumulative lifelong exposure is the strongest factor.
- Pre-malignant skin lesions: actinic keratosis, leukoplakia.
- Chronic inflammation or scars (e.g. Marjolin’s ulcer in burns or ulcers).
- Ionising radiation, tar, soot, oils, smoking, arsenic exposure.
- Immunosuppression - organ transplant patients, HIV.
- Increasing age due to cumulative DNA damage.
👀 Clinical Features
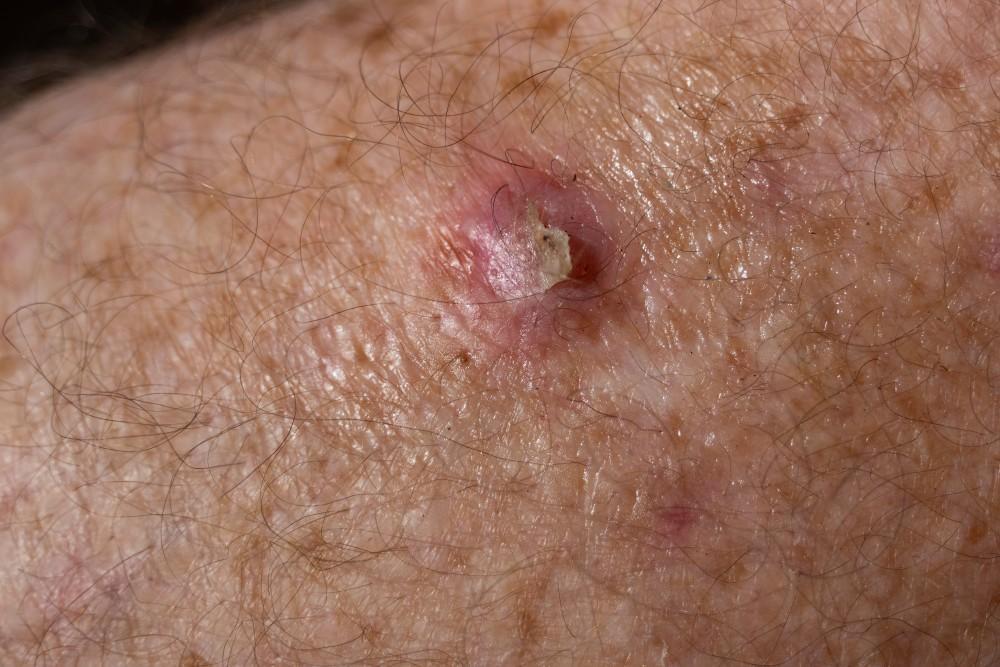
- Non-healing ulcer or crusted, scaly nodule with a firm, indurated edge.
- Most often on face, lips, ears, scalp, and hands.
- May bleed, crust, or become painful.
- Advanced disease → invasion of deeper tissue, perineural spread, or metastasis to lymph nodes.
- High-risk SCC: lesions on lip/ear, diameter >2cm, depth >4mm, poorly differentiated histology, or in immunosuppressed patients.
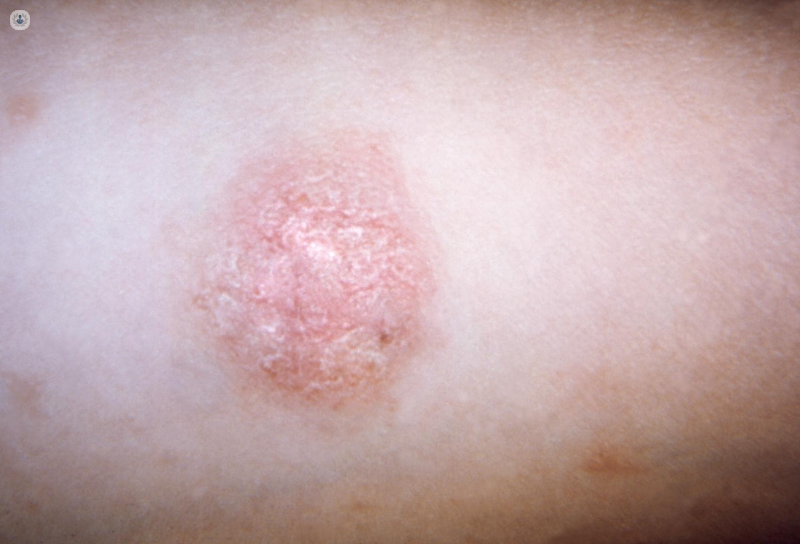
🧩 Bowen’s Disease
- Bowen’s disease = SCC in situ (confined to the epidermis).
- Presents as a scaly, erythematous plaque resembling psoriasis or eczema but persistent.
- 10–20% risk of progression to invasive SCC if untreated.
🧪 Investigations
- Skin biopsy - diagnostic, showing atypical squamous cells invading dermis.
- Lymph node assessment - FNA or biopsy if palpable.
- Imaging (CT/MRI) - advanced or high-risk lesions.
💊 Management
- Bowen’s disease:
- Curettage + cautery, cryotherapy, or photodynamic therapy.
- Topical 5-fluorouracil or imiquimod may be used.
- Invasive SCC:
- Surgical excision with adequate margins (4–6 mm for low-risk, wider for high-risk).
- Mohs micrographic surgery - best for cosmetically sensitive or recurrent lesions (lips, eyelids, nose).
- Radiotherapy - option for inoperable cases or adjuvant in high-risk SCC.
- Systemic therapy: Rare; immunotherapy (e.g., PD-1 inhibitors like cemiplimab) in metastatic/unresectable SCC.
- Follow-up: Every 3–6 months initially, due to risk of recurrence and new primary tumours.
🔮 Prognosis
- Early-detected SCC has an excellent prognosis.
- 5-year survival >90% if localised, but lower with nodal/distant spread.
- High-risk lesions need closer surveillance and MDT input.
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
