| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Immune Reconstitution Syndrome
Related Subjects: |AIDS (HIV) Neurological Disease |AIDS (HIV) Respiratory disease |AIDS Dementia Complex (HIV) |AIDS HIV Infection |AIDS(HIV) Gastrointestinal Disease |Acute Retroviral Syndrome (HIV) |HIV and Post-Exposure Prophylaxis (PEP) |HIV and Pre-exposure prophylaxis |HIV associated nephropathy (HIVAN) |HIV disease Assessment |Immune Reconstitution Syndrome
🌐 Immune Reconstitution Inflammatory Syndrome (IRIS) is an exaggerated inflammatory response seen after starting ART. It can “unmask” or worsen infections like Mycobacterium avium intracellulare (MAI) or tuberculosis. Lymphadenitis with node enlargement may evolve over weeks, often mimicking infection reactivation.
📖 About
- Occurs after initiation of HAART (Highly Active Antiretroviral Therapy).
- Driven by rapid immune recovery: ↑ CD4 T-cells, ↓ viral load → overactive immune response against latent pathogens.
- Most common in patients with baseline CD4 < 50 cells/mm³.
- Two patterns:
- 💡 Unmasking IRIS → latent infection becomes clinically apparent.
- 💡 Paradoxical IRIS → worsening of a known infection after ART.
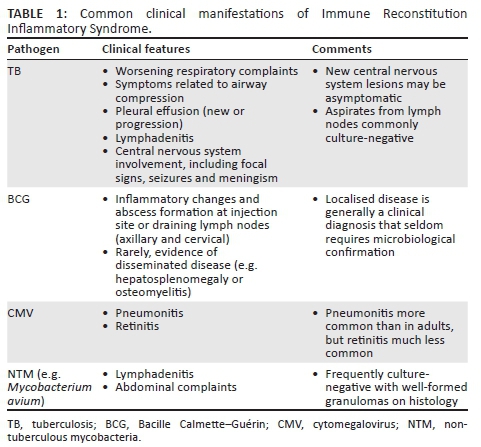 ⚠️ Clinical Features
⚠️ Clinical Features
- 🌡️ Systemic: fever, malaise, headache, night sweats.
- 🦠 Lymphadenitis: enlarged, tender nodes (esp. MAI or TB related).
- 👁️ Worsening of CMV retinitis → can threaten vision.
- Opportunistic infections flaring: PCP, Cryptococcus, Toxoplasmosis.
- Herpesvirus reactivation: CMV, HSV, varicella-zoster.
- Neurological: deterioration of PML (JC virus) after ART initiation.
- Symptoms often start within 2–12 weeks of ART commencement.
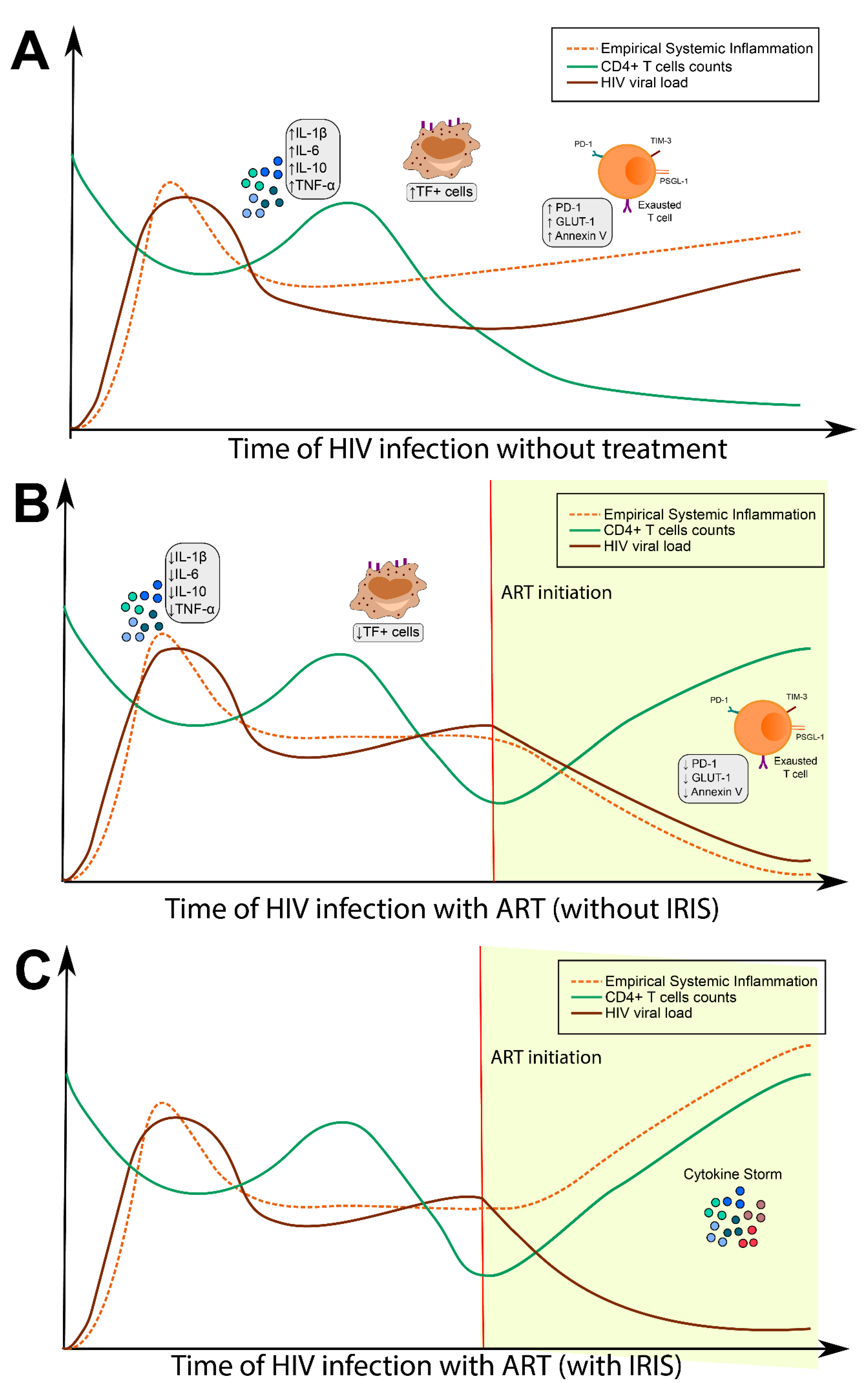 🔎 Investigations
🔎 Investigations
- 🧪 Lymph node biopsy: granulomas, acid-fast bacilli (MAI or TB).
- Bloods: ↑ liver enzymes (esp. with HBV/HCV co-infection), ↑ CRP/ESR.
- Microbiology: cultures for TB, MAI, Cryptococcus, toxoplasmosis as indicated.
- Neuroimaging if neurological features → exclude PML, toxoplasmosis.
🌀 Complications
- Severe inflammatory damage to organs (lung infiltrates, CNS lesions).
- Visual loss from CMV retinitis flare.
- Respiratory compromise (PCP/MAI lung disease).
- Neurological decline (PML progression).
🛠️ Management
- 🔑 Continue ART (unless life-threatening IRIS).
- 🎯 Treat the underlying infection aggressively (e.g. anti-TB therapy, MAI regimen with clarithromycin/ethambutol).
- 💊 Corticosteroids: consider in severe IRIS with mass effect, CNS involvement, or severe systemic symptoms.
- Supportive care: antipyretics, analgesia, manage complications (e.g. O₂ for respiratory distress).
- Multidisciplinary input: HIV physician, microbiology/ID, ophthalmology (for CMV), neurology (for CNS disease).
📚 References
Cases - Immune Reconstitution Inflammatory Syndrome (IRIS)
- Case 1 - TB-Associated IRIS: A 34-year-old man with advanced HIV (CD4 count 45) starts antiretroviral therapy (ART) while on treatment for pulmonary TB. Four weeks later he develops worsening fever, cough, and enlarging cervical lymphadenopathy despite good adherence to TB therapy. Diagnosis: Paradoxical TB-associated IRIS. Management: Continue both ART and TB therapy; add corticosteroids for severe inflammation; monitor closely for airway compromise.
- Case 2 - Cryptococcal IRIS: A 29-year-old woman with HIV begins ART after treatment for cryptococcal meningitis. Two months later, she presents with recurrent headache, fever, and raised intracranial pressure, but CSF culture is sterile. Diagnosis: Cryptococcal IRIS. Management: Continue ART and antifungal therapy; manage raised intracranial pressure (serial lumbar punctures); corticosteroids if life-threatening.
Teaching Commentary 🧬
IRIS occurs when a recovering immune system mounts an excessive inflammatory response to existing infections after ART initiation. It is most often seen with TB, cryptococcosis, CMV, and Mycobacterium avium. There are two patterns: - Paradoxical IRIS: worsening of a known, previously treated infection. - Unmasking IRIS: new presentation of a previously subclinical infection. Management principles: continue ART and infection-specific therapy; use corticosteroids for severe or life-threatening cases; supportive care. Prevention includes delaying ART initiation in cryptococcal meningitis until infection is controlled.
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
