| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Metabolic acidosis
Related Subjects: |Metabolic acidosis |Aspirin or Salicylates toxicity |Ethylene glycol toxicity |Renal Tubular Acidosis |Lactic acidosis |Metabolic alkalosis
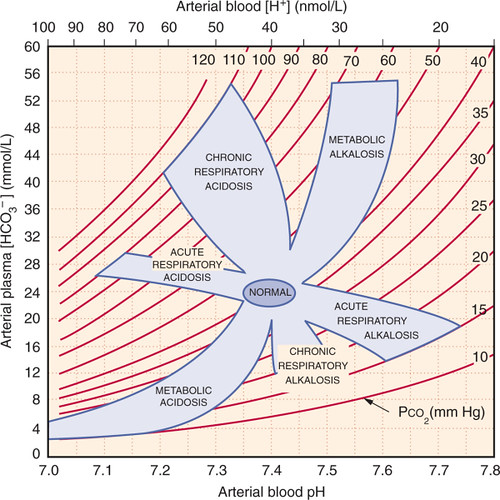
🧪 Analysis of Metabolic Acidosis (ABG)
- pH < 7.35 (unless compensated).
- HCO₃⁻ < 22 mmol/L.
- PaCO₂ usually low (<5.3 kPa) due to respiratory compensation (hyperventilation).
- PaO₂ often normal.
- Base Excess < -2.
⚡ Aetiology
- Accumulation of organic or inorganic acids.
- Loss of bicarbonate (HCO₃⁻).
- Anion Gap (AG) = (Na⁺ + K⁺) – (Cl⁻ + HCO₃⁻). Normal = 8–12 mmol/L.
📊 Causes by Anion Gap
| 🔺 High Anion Gap | ➡️ Normal Anion Gap |
|---|---|
|
|
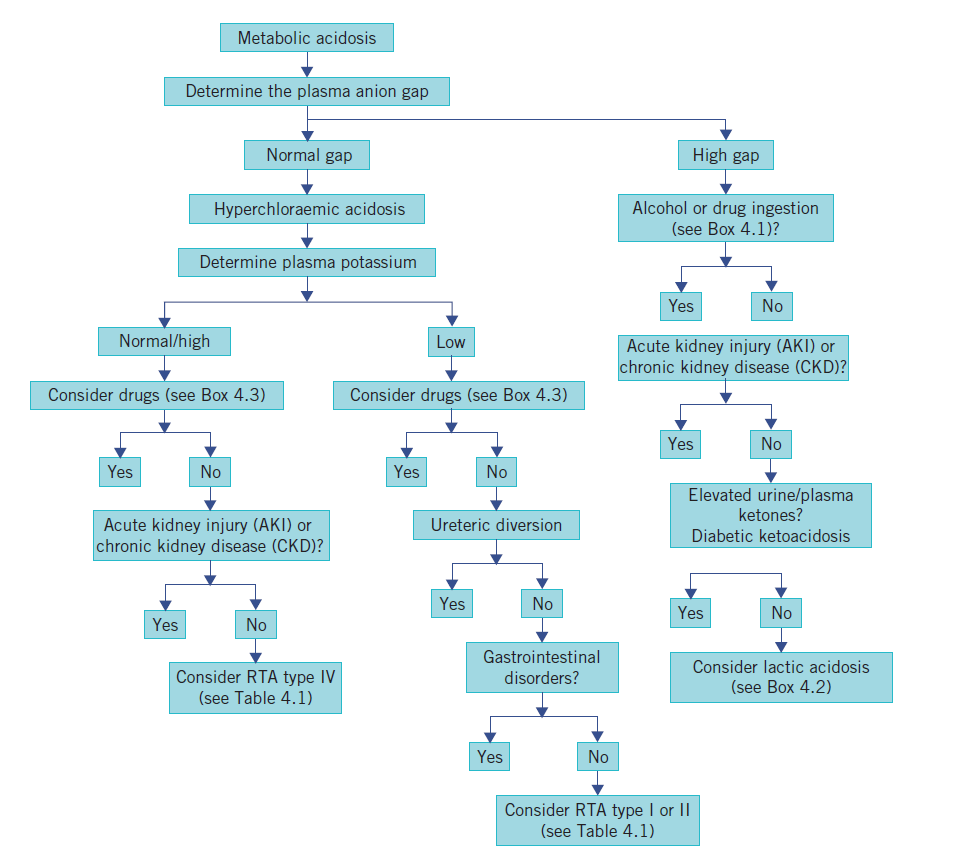
🧠 Clinical Features
- Hyperventilation (Kussmaul breathing).
- Underlying cause often obvious (shock, DKA, diarrhoea etc.).
- AG helps narrow differential.
🔎 Key Anion Gap Markers
| Anion | Clinical Case |
|---|---|
| 🧪 L-Lactate | Anaerobic metabolism (shock, sepsis). |
| 🍩 Beta-hydroxybutyrate | Diabetic ketoacidosis. |
| 🧴 Hippurate | Toluene poisoning (glue sniffers). |
| 🥛 Glycolate & Oxalate | Methanol/ethylene glycol ingestion. |
| 🌿 D-Lactate | Gut fermentation (e.g., blind loop syndrome). |
💊 Management by Cause
| Cause | Clinical Features | Diagnostic Tests | Management |
|---|---|---|---|
| 💉 Lactic Acidosis | Shock, sepsis, hypoxia, confusion, tachypnoea. | ABG (low pH/HCO₃⁻), serum lactate ↑. | Oxygen, IV fluids, treat cause, inotropes (noradrenaline if septic shock). |
| 🍩 Ketoacidosis | Polyuria, polydipsia, fruity breath, dehydration, confusion. | ABG (low pH, low HCO₃⁻), ketones ↑, glucose ↑ (DKA). | IV fluids, insulin infusion (if DKA), K⁺ replacement, monitor glucose & ketones. |
| 🩺 Renal Failure | Oedema, oliguria, confusion, uremia. | Creatinine ↑, urea ↑, ABG acidosis, electrolytes (hyperkalaemia). | Dialysis if severe, correct underlying cause, treat K⁺ imbalance. |
| ☠️ Toxins | Visual loss (methanol), renal failure (ethylene glycol), tinnitus (salicylates). | ABG: HAGMA, osmolar gap ↑, toxin assays. | Fomepizole, dialysis, bicarbonate (salicylates). |
| 💩 Diarrhoea | Loose stools, dehydration, cramps, lethargy. | ABG: NAGMA, low K⁺, low Na⁺. | Rehydrate (oral/IV), replace electrolytes, treat cause (infection, malabsorption). |
| ⚡ Renal Tubular Acidosis | Polyuria, weakness, bone pain, growth delay (children). | ABG: NAGMA, urine pH pattern, electrolytes. | Oral bicarbonate (NaHCO₃ or K-citrate), treat cause. |
| 🧂 Hyperchloremic Acidosis | Weakness, confusion, oedema if fluid overload. | ABG: NAGMA, Cl⁻ ↑, HCO₃⁻ ↓. | Stop saline infusion, use balanced fluids (Hartmann’s/Ringer’s), correct electrolytes. |
🩺 Case 1 - Diabetic Ketoacidosis (DKA)
A 24-year-old woman with type 1 diabetes presents with abdominal pain, vomiting, and drowsiness. Vitals: HR 120, BP 95/60, RR 28 with Kussmaul breathing. Labs: glucose 28 mmol/L, ketones 6 mmol/L, pH 7.15, HCO₃⁻ 10 mmol/L. Management: 💉 Fixed-rate IV insulin infusion, IV fluids (0.9% saline initially), potassium replacement as guided, identify trigger (infection). Avoid: ❌ Bicarbonate therapy unless pH <6.9; avoid rapid fluid shifts in young patients (risk of cerebral oedema).
🩺 Case 2 - Lactic Acidosis in Sepsis
A 68-year-old man presents with fever, hypotension, and confusion. BP 80/50, HR 120, lactate 6.2 mmol/L, pH 7.22, HCO₃⁻ 14 mmol/L. Diagnosis: septic shock with lactic acidosis. Management: 🚑 Sepsis 6 bundle - IV fluids, broad-spectrum antibiotics, oxygen, source control. Consider vasopressors if hypotension persists. Avoid: ❌ Delaying antibiotics; avoid excessive normal saline (can worsen acidosis with hyperchloraemia).
🩺 Case 3 - Renal Failure (Uraemic Acidosis)
A 75-year-old woman with stage 5 chronic kidney disease presents with progressive weakness, nausea, and confusion. Labs: pH 7.28, HCO₃⁻ 16 mmol/L, high urea and creatinine, potassium 6.0 mmol/L. Management: 🩺 Sodium bicarbonate therapy if symptomatic and not fluid overloaded, treat hyperkalaemia, dialysis if severe or refractory. Avoid: ❌ Relying on IV fluids alone; avoid potassium-sparing drugs (e.g. spironolactone, ACEI) in the acute setting.
Categories
- A Level
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Gynaecology
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neu
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- OSCEs
- Obstetrics
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Renal
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
