| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Ventricular Tachycardia VT ✅
Related Subjects: |Electrical Storm (Recurrent VT/VF) |Ventricular Fibrillation |Classical Ventricular Tachycardia |Idiopathic Ventricular Tachycardia |Resuscitation - Adult Tachycardia Algorithm |Resuscitation - Advanced Life Support |Automatic Implantable Cardioverter Defibrillator (AICD) |Brugada Syndrome |Long QT syndrome (LQTS) Acquired |Long QT syndrome (LQTS) Congenital |Torsades de Pointes |Wolff-Parkinson White syndrome (WPW) |Supraventricular Tachycardia (SVT) |Atrial Flutter |Atrial Fibrillation
⚡ Ensure a defibrillator is immediately available, switched on, and ready for use. Follow the Adult Tachycardia Algorithm (Resuscitation Council UK / ALS 2021).
| 📋 Management Summary: IV Access & Defibrillator Preparedness |
|---|
|
ℹ️ Key Points
- 📊 Broad-complex tachycardia (>120 bpm) usually ventricular in origin, commonly post-MI.
- ⚠️ Even seemingly stable patients can deteriorate → always prepare for rapid intervention.
- 🏥 Admit to CCU / high-dependency unit; continuous ECG monitoring and immediate defibrillator access required.
📌 Types of VT
- Sustained VT: ≥30 seconds or requiring intervention due to haemodynamic compromise.
- Non-sustained VT: ≥3 consecutive ventricular beats, lasting <30 seconds, rate >100 bpm.
🩺 Causes of VT
- ❤️ Ischaemic cardiomyopathy (most common)
- 💪 LVH (e.g., hypertension)
- 🫀 Idiopathic dilated cardiomyopathy
- ⚡ Channelopathies: Brugada syndrome, long QT syndromes
- 🧬 ARVC (Arrhythmogenic Right Ventricular Cardiomyopathy)
- 🦠 Myocarditis
- 🏋️ Hypertrophic cardiomyopathy
- 💊 Drugs / toxins: TCAs, digoxin, antiarrhythmics, cocaine
- 🧪 Electrolyte disturbances: hypo-/hyperkalaemia, hypomagnesaemia
- 💉 Phaeochromocytoma
- ➡️ RVOT VT (LBBB morphology + RAD)
👨⚕️ Clinical Presentation
- Palpitations, dizziness, syncope
- 💨 Pulmonary oedema, 🩸 hypotension, chest pain
- JVP: cannon a-waves possible
- Sudden cardiac arrest in severe cases
📈 ECG Features
- Wide QRS complex >120 ms
- AV dissociation, fusion/capture beats
- Extreme axis deviation or RS absence in precordial leads
- Monomorphic vs polymorphic (torsades de pointes: polymorphic, twisting QRS around baseline)
12-Lead ECG - Ventricular Tachycardia
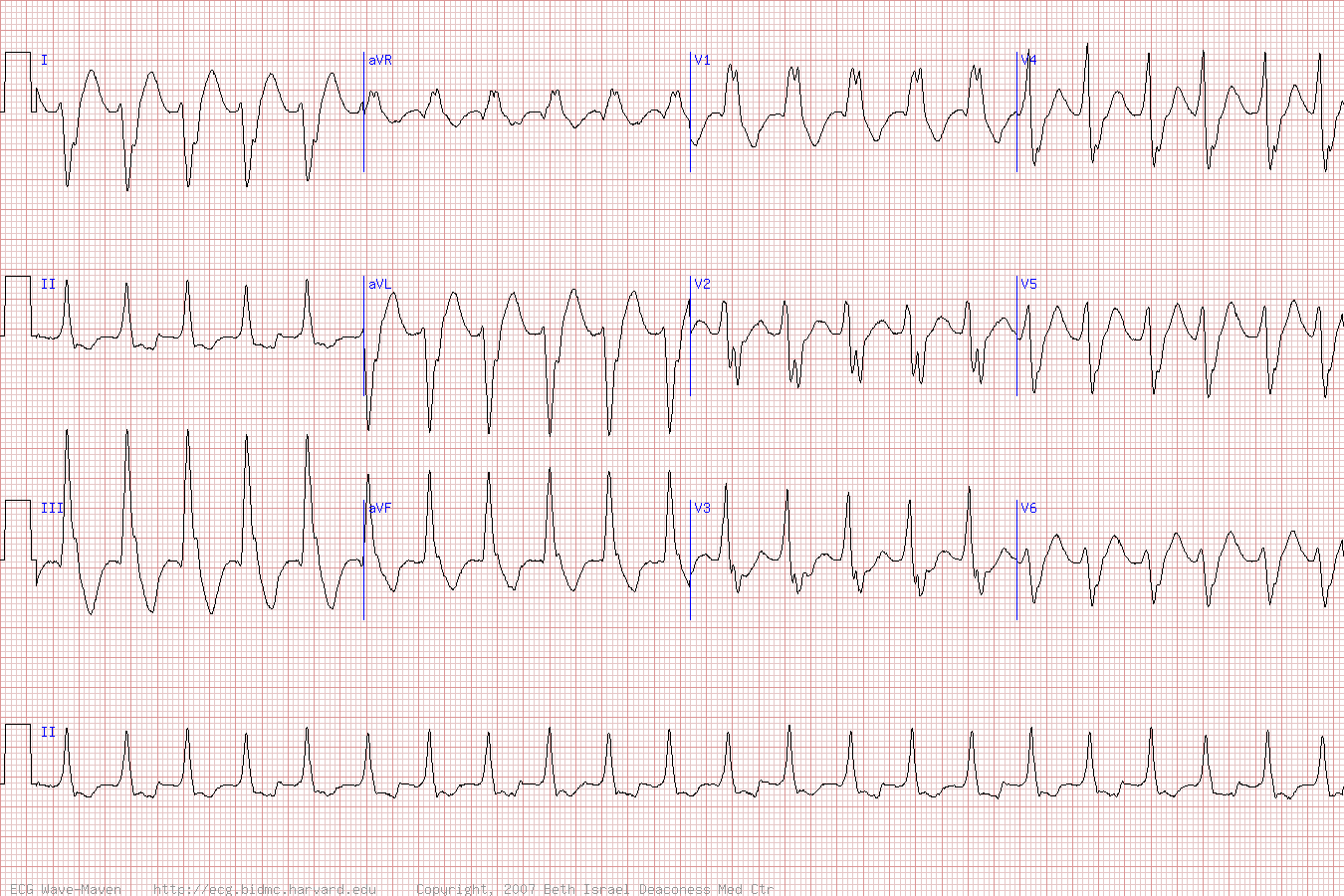
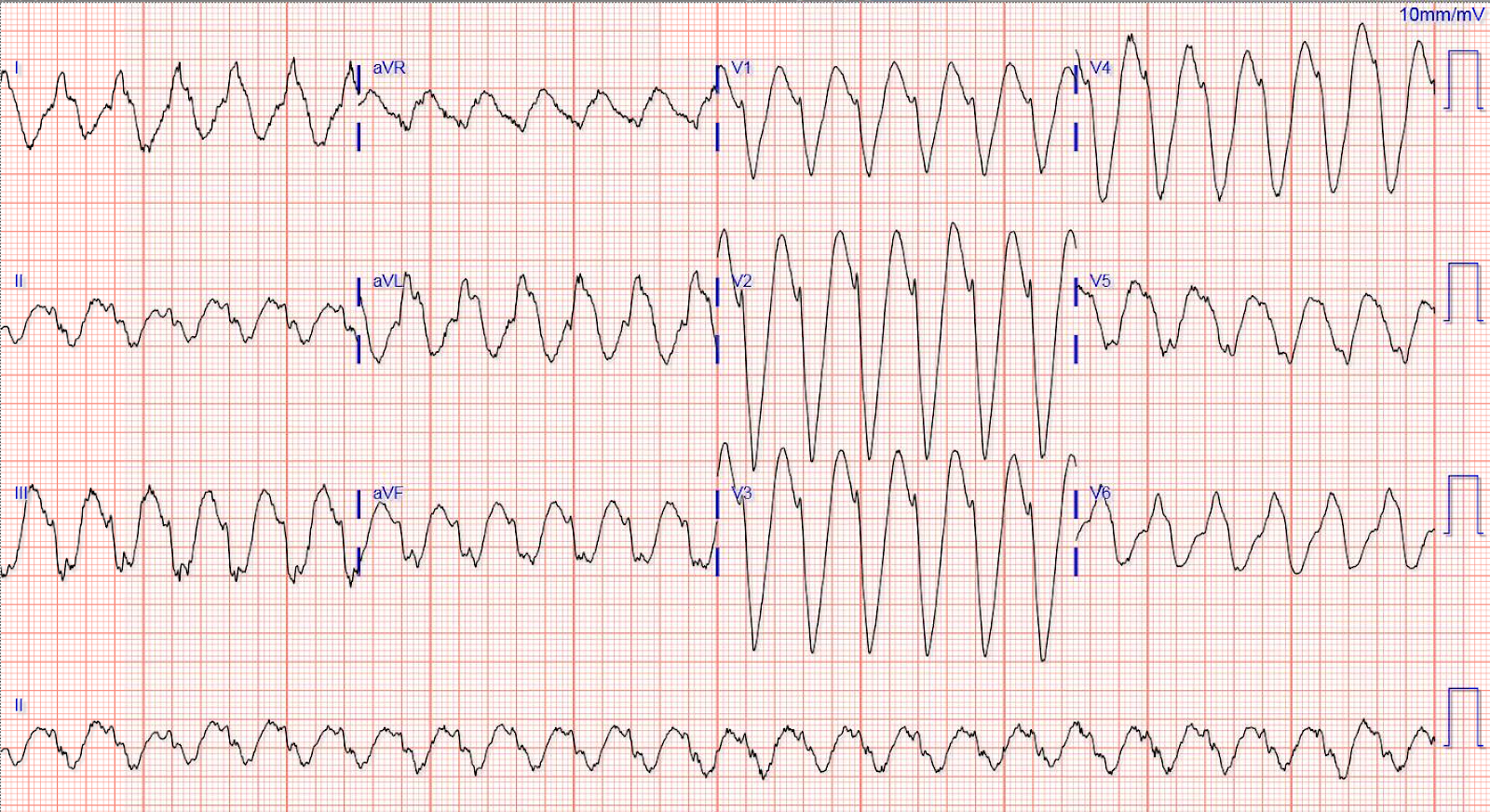
🔀 Differential Diagnosis of Regular Wide-Complex Tachycardia
- ⚡ Ventricular Tachycardia (assume VT if unsure)
- ↔️ SVT with bundle branch block
- ↔️ Atrial flutter with BBB
- 🧪 Severe hyperkalaemia
- ⚡ Pre-excited atrial tachycardia (WPW)
🧪 Investigations
- Bloods: FBC, U&E, Mg²⁺, Ca²⁺, lactate, ABG, troponin
- ECG: continuous monitoring, 12-lead for diagnosis
- Echocardiography: assess LV function, structural disease
- Coronary angiography if ACS suspected
🚑 Acute Management (NICE/RCUK ALS Compliant)
- ABC assessment; pulseless → CPR + defibrillation per ALS
- Unstable VT → immediate synchronized cardioversion
- Stable VT → IV antiarrhythmics (amiodarone first-line; lidocaine or procainamide alternatives)
- Torsades de pointes → IV magnesium sulfate 2 g over 15 min; correct K⁺, Mg²⁺, Ca²⁺; temporary pacing if recurrent
- Treat reversible causes: ACS, electrolyte imbalance, hypoxia, drug toxicity
🩺 Long-Term Management
- Beta-blockers for non-sustained VT in structurally normal hearts
- EF <35–30% → consider ICD/AICD for primary prevention
- Antiarrhythmic therapy guided by cardiology/EP team
- Catheter ablation for recurrent, symptomatic VT
- Regular follow-up with ECG, Holter, and echocardiography
⚡ Ventricular Tachycardia Management Flowchart (RCUK/NICE Compliant)
→ CPR + Defibrillation (ALS algorithm)
→ Treat reversible causes (H’s & T’s)
→ Assess haemodynamic stability
- IV access, oxygen, ECG
- Correct electrolytes & reversible causes
- IV Amiodarone 5 mg/kg over 20–60 min (max 300 mg)
- Continuous monitoring, admit to CCU
- Signs: Low BP, shock, syncope, angina, acute HF
- Immediate synchronized DC cardioversion (100–200 J biphasic)
- Conscious → sedation if possible
- Post-shock → IV amiodarone if VT persists
- IV Magnesium sulfate 2 g over 15 min
- Correct K⁺, Mg²⁺, Ca²⁺
- Stop QT-prolonging drugs
- Temporary pacing if recurrent / symptomatic
🩺 Long-Term / Secondary Prevention
- Beta-blockers for non-sustained VT in structurally normal hearts
- EF <35–30% → ICD / AICD for primary prevention
- Antiarrhythmic therapy under cardiology / EP guidance
- Catheter ablation for recurrent VT
- Regular follow-up: ECG, Holter, echocardiography
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
