Cardiac Arrest in Pregnancy
Related Subjects:
|Obstetric definitions
|Diabetes and Pregnancy
|Caesarean Section (CS)
|Epilepsy in Pregnancy
|Resuscitation - Obstetric Cardiac Arrest
|Normal Labour
|Premature Labour
|Ectopic Pregnancy
|Acute Fatty Liver of Pregnancy
|Multiple Pregnancy
|Prescribing in Pregnancy
|Termination of Pregnancy (Abortion)
|VTE DVT PE in Pregnancy
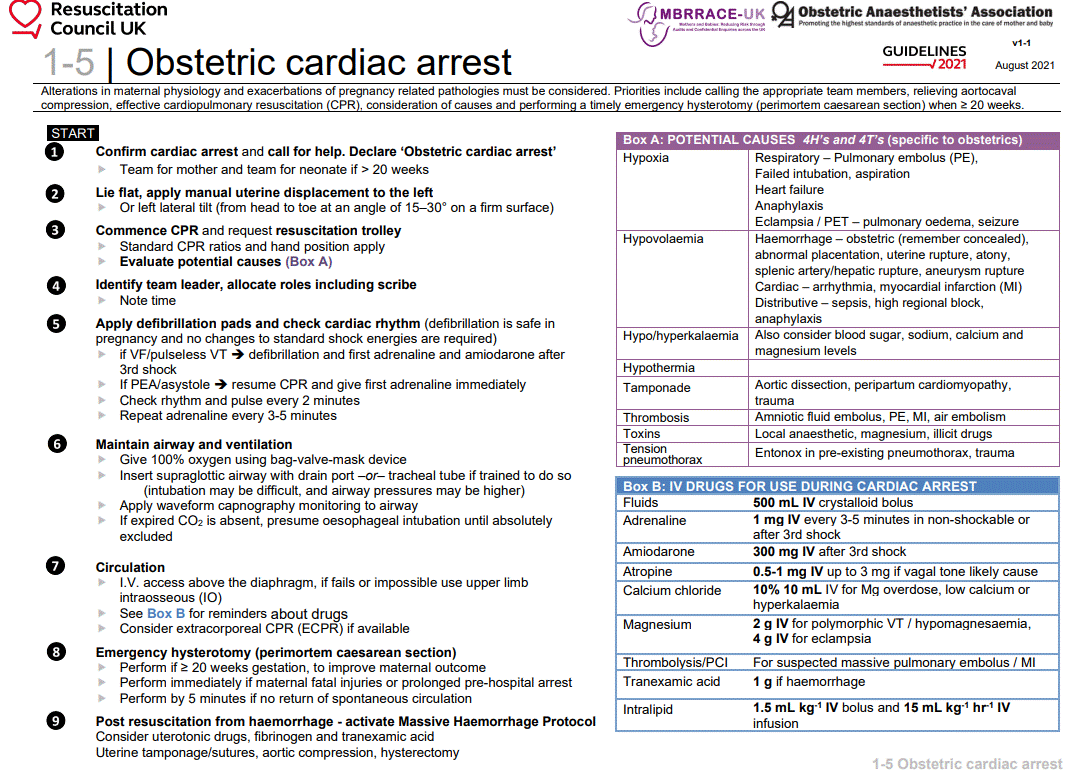
🚨 Cardiac Arrest in Pregnancy
Emergency Priorities (mother-first, UK ALS modifications)
| Priority |
Action |
Why / How |
| 🧍♀️ LUD / Tilt |
Manual left uterine displacement in supine; use 15–30° tilt only if LUD not feasible. |
Relieves aortocaval compression → improves venous return & cardiac output. Keeps compressions effective. |
| 🫁 Airway |
Early intubation + 100% O₂; plan RSI with smaller ETT (6.5–7.0); use continuous capnography. |
Pregnancy causes airway oedema & rapid desaturation. Aim for first-pass success; avoid hypo-/hyperventilation. |
| ❤️ CPR & Defib |
Standard ALS (defib energies & drugs unchanged). Hand position slightly higher on sternum; compress at 100–120/min, 5–6 cm. |
Gravid uterus shifts heart cephalad; quality compressions are critical. Give adrenaline 1 mg IV every 3–5 min as per ALS. |
| 🍼 PMCD |
Perimortem C-section if no ROSC by 4 min → aim to deliver by 5 min; perform on site. |
Maternal intervention: improves venous return & CO; increases neonatal survival if ≥24 wks (fundus ≥ umbilicus ≈ ≥20 wks if uncertain). |
Maternal cardiac arrest is rare but critical. Management = standard ALS + pregnancy-specific modifications.
Saving the mother gives the fetus the best chance of survival.
⚡ Causes (Reversible – “BEAU-CHOPS”)
- 🩸 Bleeding (PPH, abruption, uterine rupture)
• Shock, vaginal bleeding, uterine tenderness.
• 🚑 Mx: ABC, massive transfusion protocol, uterotonics, surgical repair/hysterectomy.
- 🫁 Embolism (PE, amniotic fluid, air)
• Sudden collapse, hypoxia, coagulopathy (AFE).
• 🚑 Mx: O₂, ALS, thrombolysis/thrombectomy (PE), supportive fluids/vasopressors/blood products (AFE).
- 💉 Anaesthetic complications (high spinal, aspiration, anaphylaxis)
• Hypotension, hypoventilation, desaturation.
• 🚑 Mx: Intubate + 100% O₂, stop offending agent, anaphylaxis protocol (adrenaline, fluids, antihistamines, steroids).
- 🧷 Uterine atony (major PPH cause)
• Boggy enlarged uterus, postpartum haemorrhage.
• 🚑 Mx: Uterotonics (oxytocin, ergometrine, carboprost, misoprostol), uterine massage, balloon tamponade, surgery ± hysterectomy.
- ❤️ Cardiac disease (MI, arrhythmia, cardiomyopathy)
• Chest pain, palpitations, cardiac history.
• 🚑 Mx: PCI (MI), defibrillation/anti-arrhythmics, inotropes/ECMO for cardiomyopathy.
- ⚡ Hypertension (eclampsia, HELLP)
• Seizures, headache, visual changes, RUQ pain.
• 🚑 Mx: IV MgSO₄, antihypertensives (labetalol/hydralazine), expedite delivery if viable.
- 🚑 Other causes (trauma, metabolic, anaphylaxis)
• Trauma → bleeding, pelvic injury; Sepsis → fever, hypotension.
• 🚑 Mx: ATLS (trauma), IV antibiotics + source control (sepsis), adrenaline + airway support (anaphylaxis).
- 🧬 Placentation problems (previa, accreta, percreta)
• Massive obstetric haemorrhage, shock.
• 🚑 Mx: ABC, massive transfusion, surgical control ± hysterectomy, IR if available.
- 🦠 Sepsis (chorioamnionitis, puerperal sepsis, septic abortion)
• Fever, tachycardia, hypotension, confusion.
• 🚑 Mx: IV broad-spectrum antibiotics within 1 hr, fluids, vasopressors if refractory, surgical source control.
🍼 Perimortem Caesarean Delivery (PMCD)
- Start PMCD if no ROSC within 4 min → deliver by 5 min.
- Improves maternal venous return & cardiac output, plus chance of neonatal survival if ≥24 weeks.
- Perform on site during resuscitation – do not delay for theatre.
👩⚕️ Team & Logistics
- Call obstetrics, anaesthetics, neonatology, ICU early.
- Prepare neonatal resus if viable gestation (>24 wks).
- Post-ROSC → ICU + definitive management of underlying cause.
📌 Key Takeaways
- ALS with pregnancy modifications.
- Always think BEAU-CHOPS (reversible causes).
- 4–5 minute rule: PMCD if no ROSC by 4 min.
- Maternal survival = best fetal outcome.
🧭 Practical Modifications (UK ALS)
- 🤰 Prefer manual left uterine displacement (LUD) with patient supine; use 15–30° tilt only if LUD compromises compressions.
- 💓 CPR mechanics: hands slightly higher on sternum; depth 5–6 cm, rate 100–120/min; defib energies & drug doses unchanged (e.g., adrenaline 1 mg IV every 3–5 min).
- 🫁 Difficult airway: early RSI, smaller ETT (6.5–7.0), ramped position, continuous ETCO₂; avoid hypo-/hyperventilation post-ROSC.
- 🍼 PMCD trigger: if no ROSC by 4 min → incise immediately; do not transfer. If gestation uncertain, proceed when fundus ≥ umbilicus (~≥20 wks).
- 🫀 PE arrest: consider systemic thrombolysis in maternal arrest; evaluate for ECMO where available.
- ⚡ Magnesium toxicity (eclampsia Rx): treat with IV calcium if respiratory depression or arrest occurs.
📚 References

