| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Papilloedema
Related Subjects:
|Brain tumour s
|Astrocytomas
|Brain Metastases
|Tuberous sclerosis
|Turcot's syndrome
|Lhermitte Duclos Disease
|Oligodendroglioma
|Acute Hydrocephalus
|Intracranial Hypertension
|Primary CNS Lymphoma (PCNSL)
👁️ Papilloedema is swelling of the optic disc due to raised intracranial pressure (ICP).
It requires emergency referral to ophthalmology/neuro services and urgent brain imaging (including MRV/CTV to exclude cerebral venous sinus thrombosis).
The mechanism of optic nerve damage is axoplasmic flow stasis causing intraneuronal ischaemia → untreated cases risk permanent vision loss.
Assessing optic discs can be challenging. Mydriasis is not usually required, but 0.5% tropicamide can be used if necessary.
Always document if dilating drops are used.
Papilloedema = raised ICP until proven otherwise.
👉 Always do neuroimaging before lumbar puncture to avoid coning.
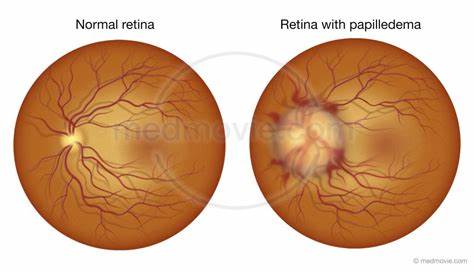
Fundoscopy: swollen disc, blurred margins, venous engorgement, haemorrhages.
Vision preserved early - differentiates from optic neuritis.
📍 About
⚠️ Causes
🔎 Pseudopapilloedema
🩺 Clinical Features
🧠 Differentials
🔬 Investigations
💊 Management
📌 Exam Tip
📚 References
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
