| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Tinea imbricata
Related Subjects: |Cellulitis |Impetigo |Pyoderma gangrenosum |Pemphigus Vulgaris |Toxic Epidermal Necrolysis |Stevens-Johnson Syndrome |Necrotising fasciitis |Gas Gangrene (Clostridium perfringens) |Anatomy of Skin |Skin Pathology and lesions |Skin and soft tissue and bone infections |Lymphangitis
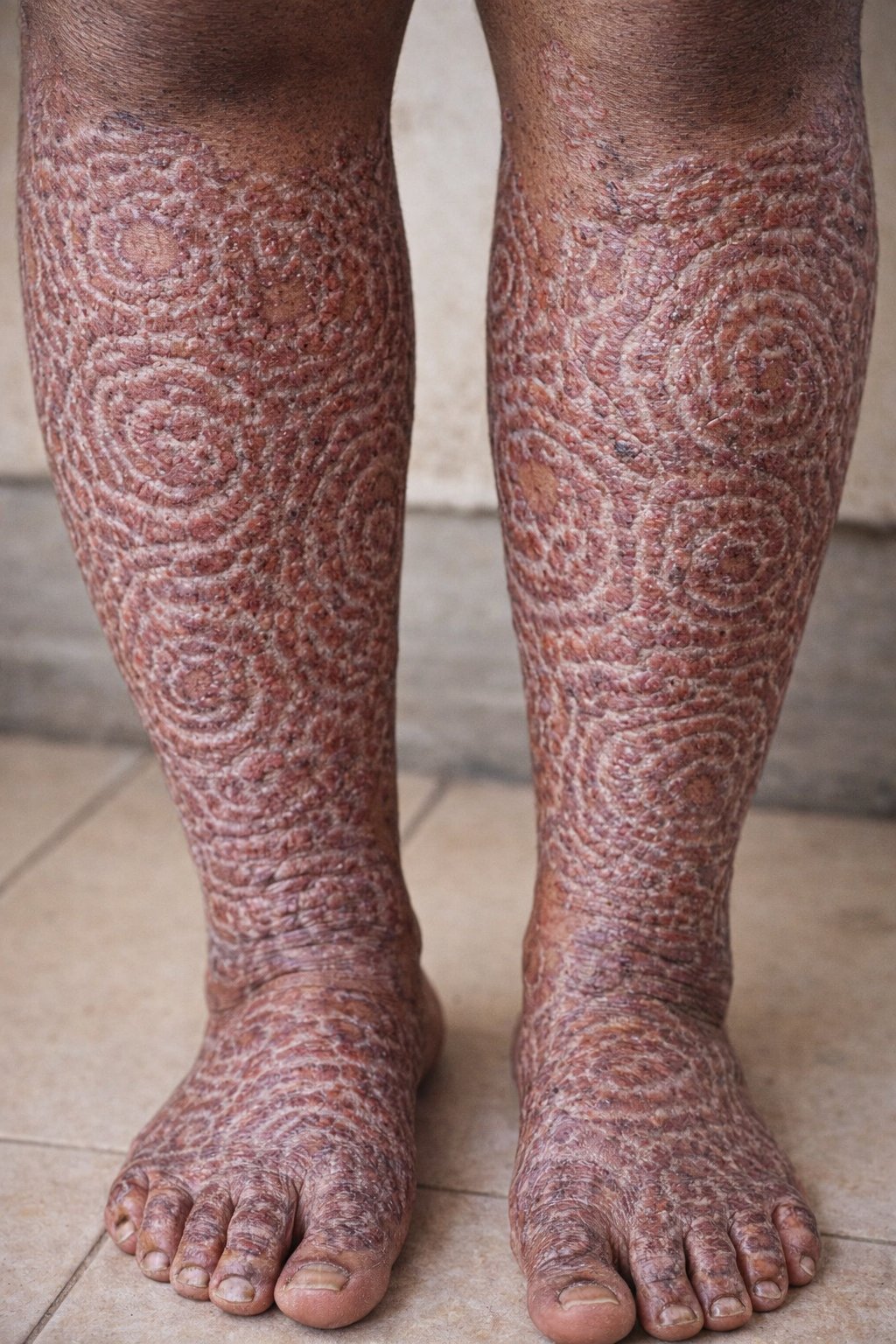
🌿 Tinea imbricata is a chronic, superficial dermatophyte infection caused by Trichophyton concentricum. 🔄 It produces characteristic concentric, overlapping rings of scale, giving a “wood-grain” or “imbricated” appearance. 🌍 It is endemic in tropical regions (Pacific Islands, Southeast Asia, Central/South America) and often reflects a degree of host immune tolerance.
📖 Definition
- A form of tinea corporis with distinctive concentric scaling rings.
- Caused specifically by Trichophyton concentricum.
🦠 Aetiology
- Dermatophyte fungus: Trichophyton concentricum
- Infection remains confined to the stratum corneum
- Associated with cell-mediated immune dysfunction (reduced response to the organism)
⚠️ Risk Factors
- 🌍 Residence in tropical/endemic regions
- 👨👩👧 Close contact / household spread
- 🧬 Genetic susceptibility (familial clustering)
- 🦠 Poor hygiene / overcrowding
🔍 Clinical Features
- 🔄 Concentric, scaly rings spreading outward
- 🎯 “Wood-grain” or imbricated pattern
- 😖 Pruritus (itching)
- 🧍 Commonly affects trunk and limbs
- ⏳ Chronic, slowly progressive course
🧪 Investigations
- 🔬 Skin scrapings + KOH microscopy → hyphae
- 🧫 Fungal culture (confirms species)
- 🧠 Diagnosis often clinical in endemic areas
💊 Management – Detailed Treatment
- ⚠️ Systemic therapy is usually required – topical treatment alone is often insufficient due to chronicity and widespread involvement.
🧴 First-line: Oral antifungals
- Terbinafine (fungicidal; inhibits squalene epoxidase)
- Adult dose: 250 mg once daily
- Duration: typically 2–4 weeks (may need longer in extensive disease)
- Advantages: high cure rates, shorter courses
- Itraconazole (fungistatic; inhibits ergosterol synthesis)
- Adult dose: 100–200 mg daily
- Duration: 2–4 weeks (longer if relapse)
- Useful alternative if terbinafine not tolerated
- Griseofulvin (older option)
- Requires longer courses (4–8 weeks+)
- Less effective and more relapse compared to terbinafine
🧴 Adjunct topical therapy
- Topical antifungals (e.g. terbinafine cream, azoles) may:
- Reduce fungal load
- Limit spread
- Improve symptoms (itching)
- 👉 Rarely sufficient as monotherapy in tinea imbricata
🧪 Monitoring & safety
- 🩸 Liver function tests (LFTs) before and during prolonged oral therapy
- ⚠️ Terbinafine and itraconazole are hepatotoxic (rare but important)
- 💊 Check for drug interactions (especially itraconazole – CYP3A4 inhibitor)
🔁 Recurrent / refractory disease
- Longer or repeated courses of oral antifungals may be required
- Consider:
- Reinfection from contacts
- Incomplete adherence
- Underlying immune tolerance
- 👉 Treat close household contacts if recurrent
🧼 Supportive & preventive measures
- 🧴 Maintain good skin hygiene
- 👕 Avoid sharing clothing/towels
- 🧼 Regular washing of clothes and bedding
- 🌿 Treat co-existing fungal infections (e.g. tinea pedis)
⚠️ Special situations
- Children: griseofulvin often preferred due to safety profile
- Pregnancy: avoid systemic antifungals where possible → specialist advice
- Immunocompromised: may need prolonged therapy and closer follow-up
🧠 Exam Tips
- 📌 “Concentric rings” = tinea imbricata (very distinctive)
- 📌 Caused by Trichophyton concentricum (unique organism)
- 📌 Often requires oral treatment (unlike simple tinea corporis)
- 📌 Seen in tropical populations → geography is a key clue
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
