| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Optic atrophy
👁️ Optic Atrophy refers to degeneration of the optic nerve, resulting in a pale optic disc and progressive vision loss. It is the end result of many optic neuropathies. Glaucoma is the most common cause worldwide, but multiple vascular, inflammatory, nutritional, and hereditary conditions can also lead to optic atrophy.
📍 About
- Represents optic nerve damage, visible as optic disc pallor on fundoscopy.
- Can follow inflammation, ischaemia, trauma, compression, toxicity, or genetic disease.
- It is a sign, not a diagnosis - always investigate the underlying cause.
🩺 Clinical Features
- Vision loss: Central or peripheral, depending on pathology.
- Colour vision changes: Subtle desaturation, often early finding.
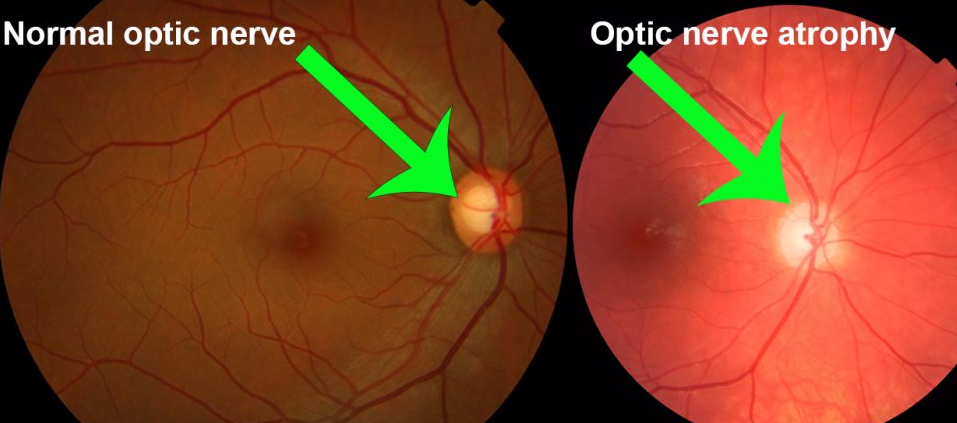
- Optic disc: Appears pale, sometimes “chalky white” in longstanding disease.
- Other associated features:
- Headache, jaw claudication, PMR symptoms → consider GCA.
- Signs of raised ICP → papilloedema progressing to atrophy.
- Relative afferent pupillary defect (RAPD) in unilateral/asymmetric cases.
🕒 Onset Patterns
- Acute (minutes–hours): Ischaemic (e.g. CRAO, AION), optic neuritis, trauma.
- Sub-acute (days): Inflammatory or infective causes.
- Chronic (weeks–months): Compression, degenerative, nutritional, toxic, glaucoma.
⚠️ Causes of Optic Atrophy
- Neurological: Idiopathic intracranial hypertension, multiple sclerosis (retrobulbar neuritis), trauma.
- Vascular: Ischaemic optic neuropathy, chronic papilloedema, temporal arteritis (GCA).
- Hereditary/Degenerative: Leber’s hereditary optic neuropathy, retinitis pigmentosa, storage diseases (e.g. Tay–Sachs).
- Toxic/Nutritional: Isoniazid, methanol, solvents; tobacco–alcohol amblyopia; vitamin B12/folate deficiency.
- Infectious/Inflammatory: Chronic optic neuritis, syphilis, TB.
- Other: Radiation, compression (tumour, aneurysm), glaucoma.
🔬 Investigations
- Blood tests:
- ESR, CRP → rule out GCA.
- Syphilis serology (FTA-ABS, RPR).
- B12 & folate levels.
- Thyroid function tests.
- CSF analysis:
- Opening pressure (after neuroimaging).
- Protein, oligoclonal bands (MS).
- Imaging: MRI/CT of orbits & brain → rule out compressive/infiltrative causes.
- Other: Toxicology screen if suspicion of toxin exposure.
💊 Management
- Treat underlying cause:
- Glaucoma: Lower intraocular pressure (drops, laser, surgery).
- GCA: Immediate high-dose steroids to protect vision.
- Nutritional deficiencies: Vitamin replacement (B12, folate).
- Infection: Targeted antimicrobials (e.g. syphilis therapy).
- Irreversible damage → supportive: low-vision aids, occupational support, counselling.
📌 Exam Tip
Always differentiate: 🔹 Disc swelling = active process (papilloedema/neuritis). 🔹 Disc pallor = established atrophy (end-stage). Unilateral optic atrophy + RAPD → think compressive lesion or optic neuritis. In an older patient with sudden vision loss + headache → rule out GCA urgently!
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
