| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
💓Atrial flutter ✅
Related Subjects: |Wolff-Parkinson White syndrome (WPW) AVRT |Lown Ganong Levine Syndrome AVRT |Supraventricular Tachycardia (SVT) |Atrioventricular Nodal Reentrant Tachycardia AVNRT |Atrial Flutter |Atrial Fibrillation |Sinus Tachycardia |Sinus Arrhythmia |Multifocal Atrial Tachycardia |Resuscitation - Adult Tachycardia Algorithm |AF and Anticoagulation
⚠️ Important: Class I antiarrhythmics (e.g. flecainide) must be used with AV nodal blockade (β-blocker or rate-limiting calcium channel blocker) to prevent dangerous 1:1 AV conduction ⚡. ❌ Avoid antiarrhythmic monotherapy in atrial flutter. 🔥 Catheter ablation (targeting the re-entrant circuit) has >90% success and is first-line definitive therapy in typical flutter.
ℹ️ About Atrial Flutter
- ⚡ Atrial rate: 280–350 bpm due to a macro-reentrant circuit.
- 🧐 Ventricular rate typically ~150 bpm with 2:1 AV block.
- 🔄 Often alternates with atrial fibrillation (AF–flutter spectrum).
- 💓 Usually originates in the right atrium (cavotricuspid isthmus-dependent circuit).
🧬 Aetiology
- 🔁 Macro-reentrant arrhythmia (classically cavotricuspid isthmus dependent).
- ❤️ Structural heart disease: IHD, hypertension, valvular disease, cardiomyopathy.
- 🌬️ Systemic triggers: COPD, hyperthyroidism, infection, alcohol (“holiday heart” 🍷).
- 🛠️ Post-cardiac surgery or prior ablation → atypical flutter.
📊 Types of Atrial Flutter
| Type | Characteristics | Clinical Notes |
|---|---|---|
| Typical (CTI-dependent) | Re-entry around tricuspid annulus via cavotricuspid isthmus | Most common; highly amenable to catheter ablation 🔥 |
| Atypical | Non–isthmus dependent circuits (often scar-related) | Seen post-surgery/ablation; requires complex mapping |
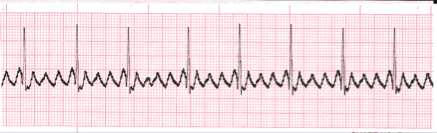
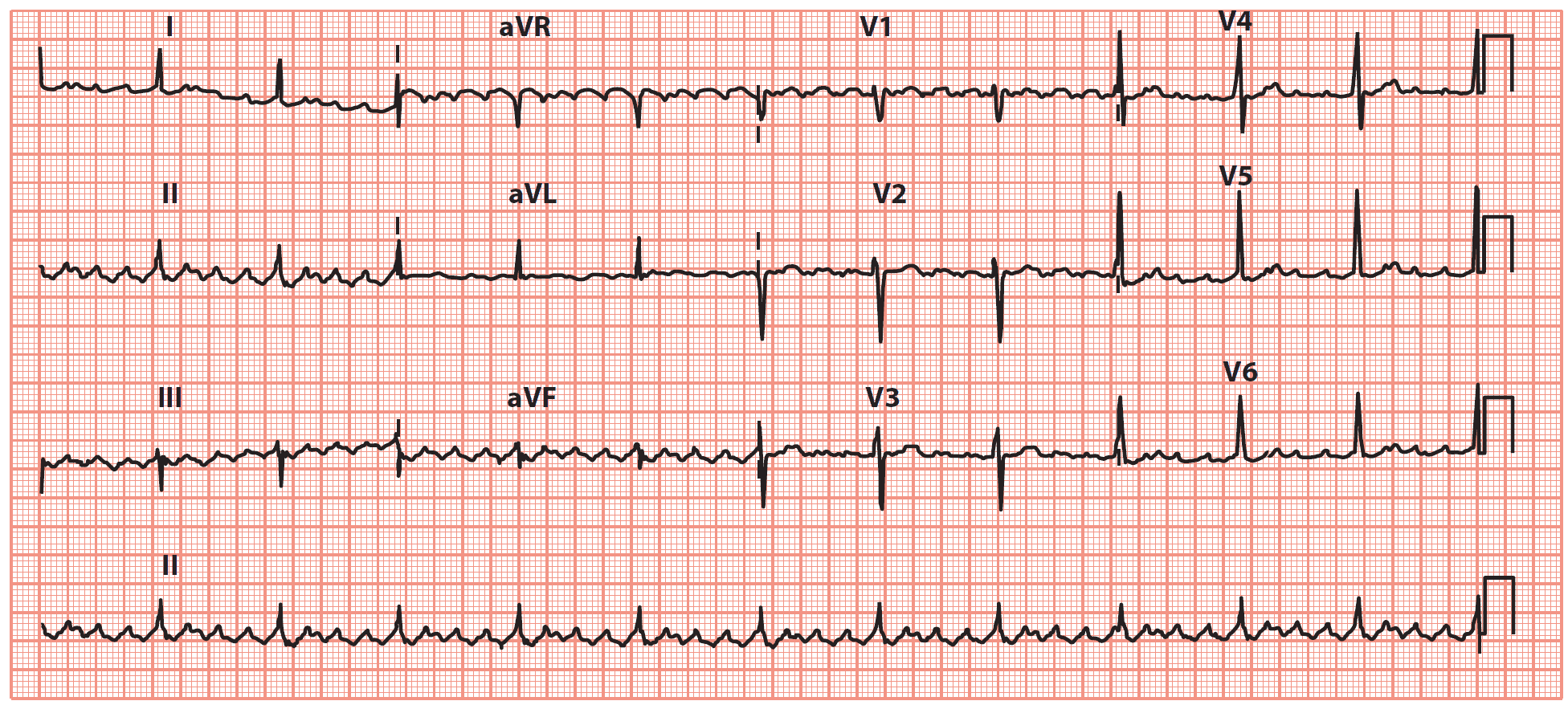
📈 ECG Findings
- 🪚 Sawtooth flutter waves, best seen in leads II, III, aVF.
- ⚡ 2:1 AV conduction → ventricular rate ~150 bpm (common).
- 🚨 1:1 conduction → ventricular rate 250–300 bpm (life-threatening).
- 💉 Adenosine or vagal manoeuvres may unmask flutter waves.

🤒 Clinical Presentation
- 💓 Palpitations, fatigue, dyspnoea, dizziness.
- 🧘 May be asymptomatic if rate controlled.
- 🚨 Severe cases: hypotension, syncope, acute heart failure.
🔬 Investigations
- 🧪 Bloods: FBC, U&E, Mg²⁺, TFTs, CRP, troponin.
- 📈 ECG: diagnostic (flutter waves + conduction pattern).
- 🩻 Echocardiography: assess LV function, atrial size, valvular disease.
- 📟 Holter monitor: paroxysmal detection.
- 💉 Adenosine: diagnostic (transient AV block reveals flutter waves).
⚡ Acute Management (NICE NG196)
- 🚨 Haemodynamically unstable: Immediate synchronized DC cardioversion.
- 🧘 Stable: Rate control first-line (β-blocker or rate-limiting CCB).
- ⏱️ Consider early cardioversion if onset <48h or patient anticoagulated.
🎛️ Rate Control
- β-blockers (e.g. bisoprolol) 👍
- Rate-limiting CCBs (diltiazem/verapamil) 👍
- Digoxin useful in sedentary patients or heart failure ⚠️ (less effective in exertion)
🔄 Rhythm Control
- ⚡ Electrical cardioversion – rapid and effective.
- 💊 Flecainide (ONLY if no structural heart disease) + AV nodal blocker.
- 💊 Amiodarone reserved for structural heart disease or refractory cases.
🔥 Catheter Ablation
- 🎯 First-line definitive therapy for typical atrial flutter.
- 📈 Success rate >90%; low recurrence.
- Reduces need for long-term antiarrhythmic drugs.
🛡️ Anticoagulation (NICE NG196)
- 📊 Use CHA₂DS₂-VASc score (same as AF).
- 💊 DOACs first-line (apixaban, rivaroxaban, dabigatran, edoxaban).
- ⚖️ Warfarin if mechanical valve or moderate–severe mitral stenosis.
- ❌ Do NOT use aspirin monotherapy for stroke prevention.
🚫 Contraindications / Caution
- ❌ Flecainide in structural heart disease or IHD.
- ❌ Non-DHP CCBs in decompensated systolic heart failure.
- ⚠️ Excess β-blockade → bradycardia, hypotension.
- ⚠️ Antiarrhythmics without AV nodal blockade → risk of 1:1 conduction ⚡
📊 Rate vs Rhythm Control
| Scenario | Preferred Strategy | Rationale |
|---|---|---|
| 🚨 Unstable | Immediate DC cardioversion | Life-saving; do not delay |
| 😷 Symptomatic stable | Rate control → consider rhythm control | Stabilise first, then restore sinus rhythm |
| 🔁 Recurrent flutter | Catheter ablation | Definitive, high success |
| 👴 Older/comorbid | Rate control + anticoagulation | Avoid drug toxicity; stroke prevention key |
🩺 Case-Based Learning
- Case 1: 66M, HR 150 → typical flutter. → β-blocker → consider cardioversion → ablation. 🧠
- Case 2: 78F, HF + flutter. → Digoxin + diuretics → anticoagulate → consider ablation. ❤️
- Case 3: 70M, HR 280, hypotensive. → 🚨 Immediate DC cardioversion. ⚡
🌱 Lifestyle & Risk Factor Management
- 🚭 Smoking cessation
- 🍷 Reduce alcohol intake
- ⚖️ Weight optimisation
- 💊 Treat HTN, thyroid disease, COPD
📚 References
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
