| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Acute and Chronic Gout ✅
Related Subjects: |Rheumatoid arthritis |Systemic Sclerosis (Scleroderma) |RA vs OA |Acute and Chronic Gout |Calcium Pyrophosphate Deposition (Pseudogout) |Hyperuricaemia |Allopurinol |Rasburicase |Lesch-Nyhan syndrome
⚠️ It is very rare for acute gout to occur in a rheumatoid joint (due to local anti-inflammatory environment). 👉 Continue treatment until 1–2 days after the attack has resolved and ensure follow-up. 🚑 Admit if septic arthritis is suspected (always exclude this via joint aspiration if possible). 📌 Remember: serum urate may be normal during an acute attack, so repeat 2+ weeks later (NICE NG219).
| Acute Gout Flare – Confirm diagnosis. Exclude Infection. Treatment (NICE NG219) |
|---|
Individualise choice (e.g. steroids preferred in CKD/cardiac disease where NSAIDs riskier). Review response in 48–72 h. Refer if refractory or diagnostic uncertainty. |
🔎 About
- Gout is the most common inflammatory arthritis, caused by deposition of monosodium urate monohydrate crystals in joints/soft tissues.
- Chronic hyperuricaemia (serum urate >360 µmol/L) leads to recurrent flares, tophi, chronic gouty arthritis, urolithiasis, and urate nephropathy.
- Common precipitants in elderly: thiazides, low-dose aspirin, ciclosporin, dehydration, alcohol binge, surgery, or dietary purines.
🧬 Aetiology
- Hyperuricaemia from overproduction (<10%; e.g., purine disorders, haematological malignancy, tumour lysis) or underexcretion (>90%; genetic, CKD, drugs).
- Crystals: needle-shaped, strongly negatively birefringent under polarised light microscopy.
- Classically affects 1st MTP joint (podagra; ~50% first attacks).
- Precipitating drugs: thiazides, ciclosporin, low-dose aspirin (<325 mg), pyrazinamide.
⚡ Effects of Hyperuricaemia
- Asymptomatic hyperuricaemia (common; no treatment unless very high risk).
- Acute gouty arthritis (mono/polyarticular flares).
- Chronic tophaceous gout (tophi, joint damage, deformity).
- Renal: urate nephrolithiasis (~20%), chronic urate nephropathy → CKD.
📊 Epidemiology
- Male predominance (M:F ≈ 3–10:1; postmenopausal women rise).
- Prevalence ~2.5–3.2% in UK adults (higher in men >40, obesity, metabolic syndrome).
- Lifestyle factors: alcohol (beer/spirits), obesity, high-purine diet (red meat, seafood), fructose-sweetened drinks.
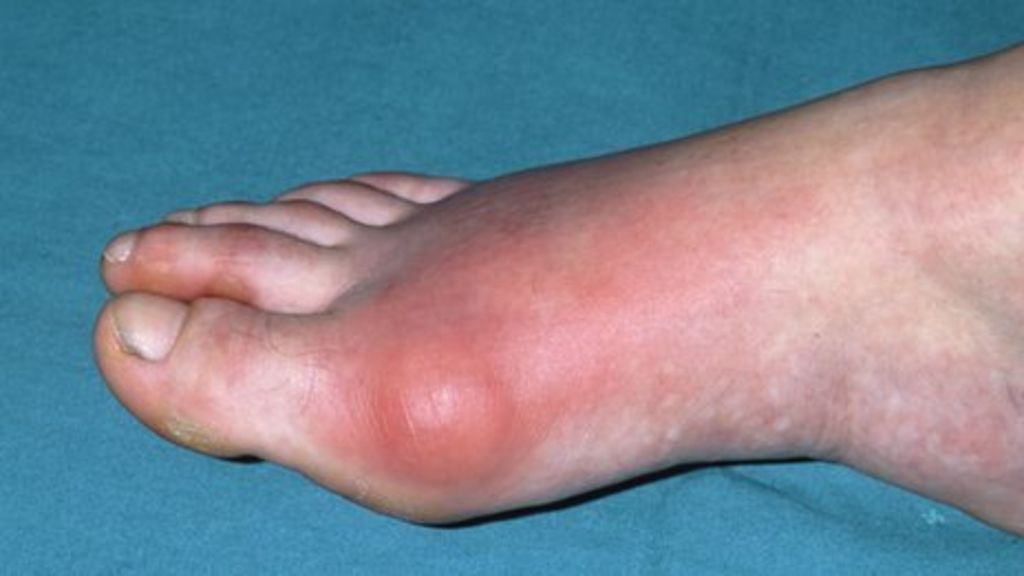
🦶 Podagra – 1st MTP joint (classic site)
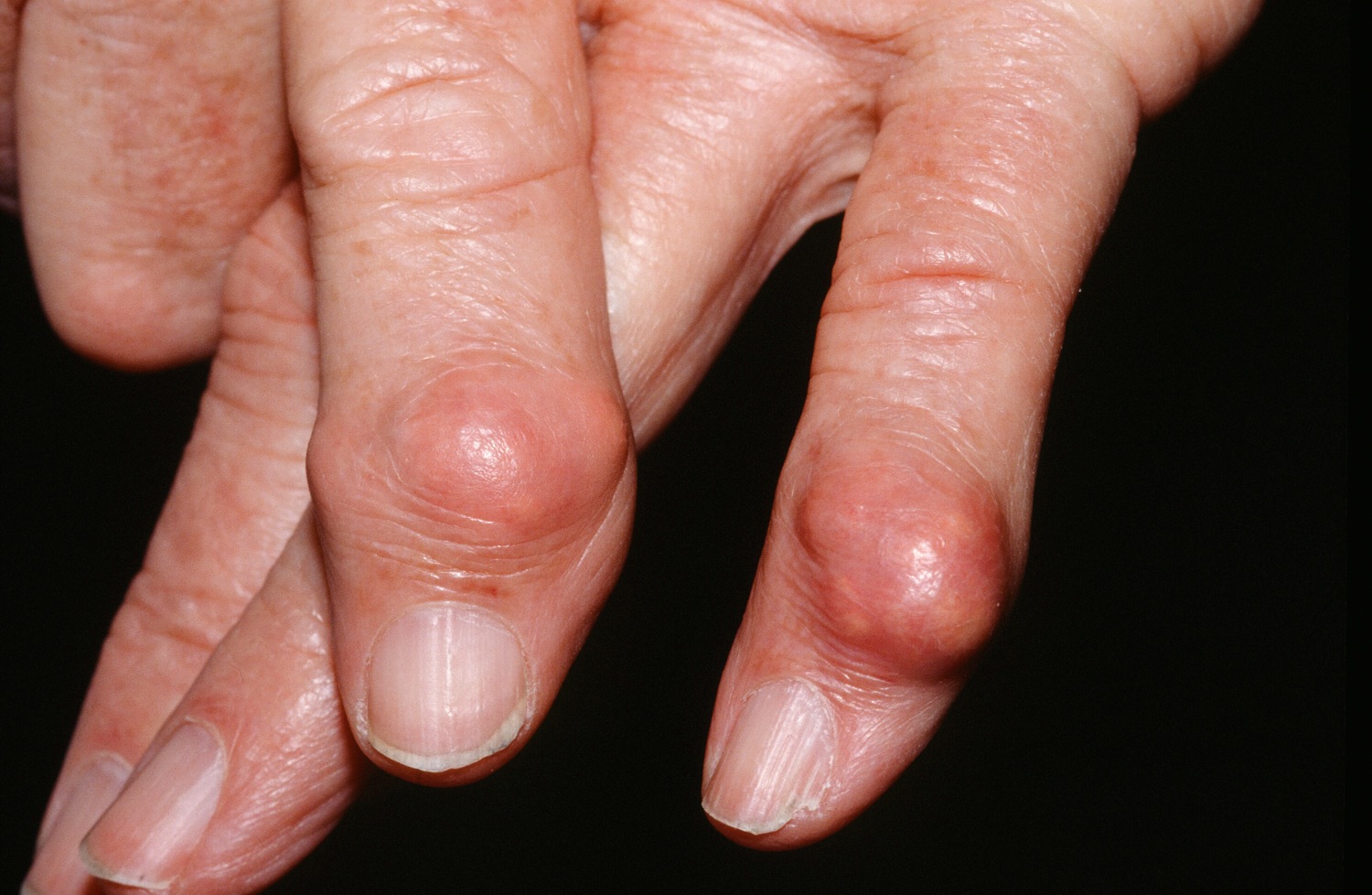
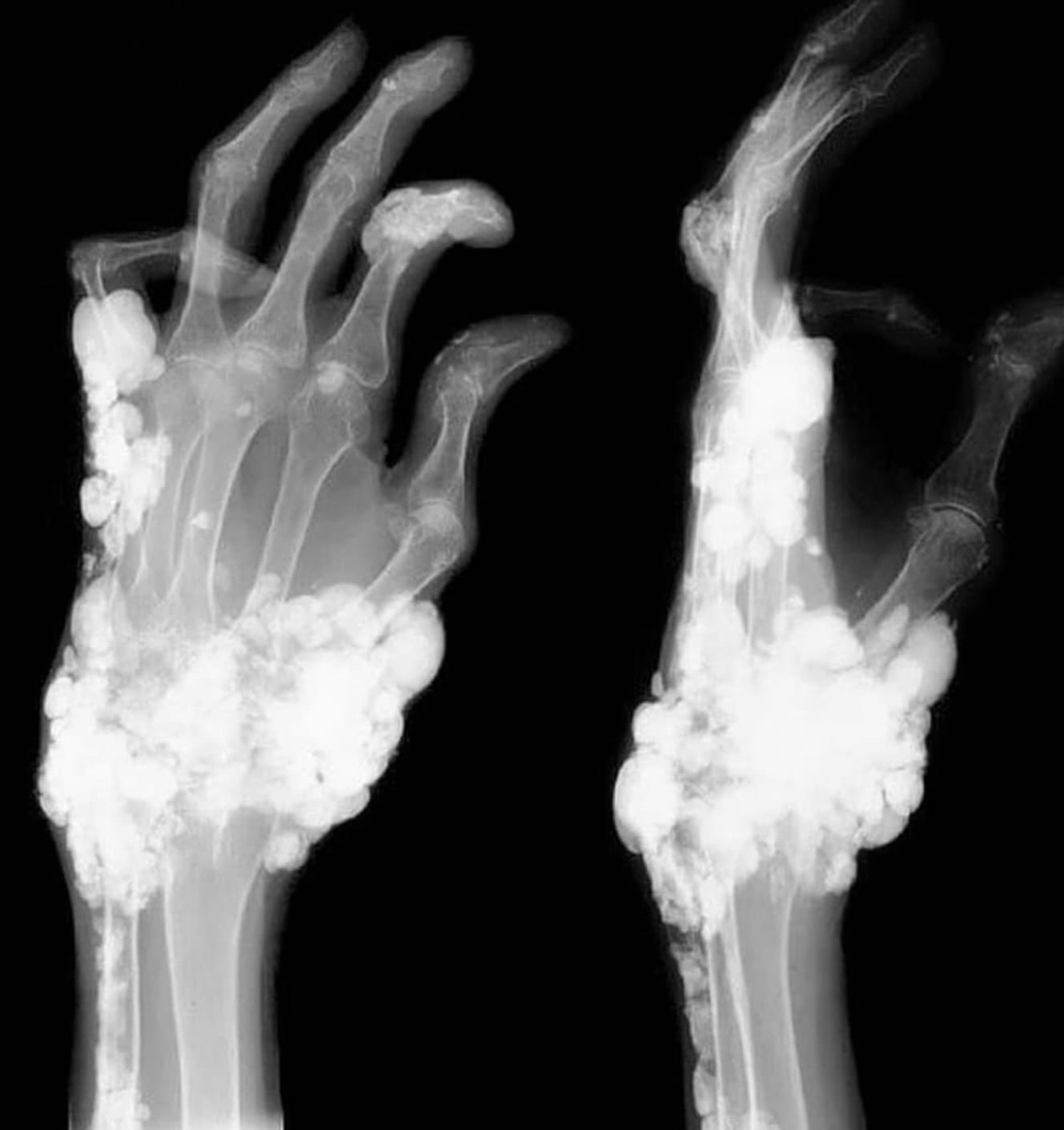
🏔️ Chronic Tophaceous Gout
🔬 Urate Crystals

⚠️ Risk Factors
- Male sex, age >40 (postmenopausal women), obesity, metabolic syndrome (hypertension, diabetes, dyslipidaemia).
- CKD, diuretics, low-dose aspirin, alcohol excess, high-purine diet.
- Genetic predisposition (e.g., SLC2A9/ABCG2 variants impair excretion).
- Rare: Lesch-Nyhan (HGPRT deficiency), tumour lysis, lead poisoning (saturnine gout).
🔺 Causes of Excess Urate
- Reduced excretion: CKD, thiazides/loop diuretics, low-dose aspirin, hypertension, lactic acidosis (alcohol/starvation), hypothyroidism, lead toxicity.
- Overproduction: HGPRT deficiency, PRPP synthetase overactivity, myeloproliferative/lymphoproliferative disorders, psoriasis, extreme exercise.
🩺 Clinical Presentation
- Sudden onset (often nocturnal), severe pain maximal in 6–12 hours, swelling, erythema, extreme tenderness (may mimic cellulitis/septic joint).
- Attack duration: 5–14 days untreated; systemic features (fever, malaise, ↑CRP/WCC).
- Polyarticular in chronic/untreated cases.
🚨 Complications
- Chronic tophi → visible/subcutaneous lumps, joint destruction/deformity, disability.
- Urate nephrolithiasis (~20%).
- Chronic urate nephropathy → progressive CKD.
🧪 Investigations (NICE NG219 Compliant)
- Bloods: FBC, U&E (CKD screen), CRP/ESR (raised in flare), serum urate (may normalise in flare → repeat ≥2 weeks post-flare).
- Joint aspiration: Gold standard (negatively birefringent needle crystals; exclude septic arthritis via Gram stain/culture).
- Radiology: Plain X-ray (punched-out erosions with overhanging edges, soft-tissue tophi); dual-energy CT (urate deposits) if available.
💊 Management (NICE NG219 Compliant)
- Acute flare: First Line. Rest, elevate, ice, analgesia.
- NSAID e.g. naproxen 500 mg BD or indomethacin 50 mg TDS + PPI if GI risk
- Colchicine low-dose: 500 µg BD–TDS (max 6 mg/course; caution diarrhoea/CKD)
- Oral corticosteroid e.g. prednisolone 15–30 mg OD for 3–5 days (no taper needed)
- Always exclude septic arthritis (aspiration if possible; admit if suspected).
- Do not stop ULT (allopurinol/febuxostat) during flare.
- Information & support: Educate on chronic nature, treatable, importance of adherence; provide written info.
- Diet & lifestyle: Advise weight loss if overweight, limit alcohol (esp. beer/spirits), avoid dehydration, reduce purine-rich foods (red meat/offal, seafood), limit sugary drinks.
- Long-term ULT:
- Offer to all with: recurrent flares (≥2/year), tophi, chronic gouty arthritis, joint damage, CKD ≥3, urolithiasis, or very high urate.
- Treat-to-target: Start low-dose allopurinol (100 mg OD; lower in CKD) or febuxostat (80 mg OD); titrate to target serum urate <360 µmol/L (<300 µmol/L if tophi/chronic damage).
- Prophylaxis: Colchicine (or NSAID/low-dose steroid) for ≥3–6 months when initiating ULT to prevent mobilisation flares.
- Febuxostat if allopurinol intolerant/fails; pegloticase (IV uricase) for severe refractory tophaceous gout (specialist only).
- Monitoring: Serum urate every 4 weeks during titration, then 6-monthly; renal function; flares/tophi.
- Referral to specialist: Diagnostic uncertainty, refractory gout, severe tophaceous disease, CKD complicating management.
📚 References (Current as of March 2026)
- NICE NG219 – Gout: diagnosis and management (2022; current)
- BSR Guideline for the Management of Gout (2017; complementary but superseded in UK by NG219)
- ACR 2020 Guideline for the Management of Gout (complementary international reference).
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Education
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Paediatrics
- Palliative
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
