| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Neurofibromatosis Type 2
Related Subjects: |Neurofibromatosis Type 1 |Neurofibromatosis Type 2 |Tuberous sclerosis |Café-au-lait spots |McCune Albright syndrome
There are at least two mechanisms for secondary hypertension in patients with Neurofibromatosis Type 2 (NF2) - Phaeochromocytoma and Renal artery stenosis.
ℹ️ About
- Neurofibromatosis Type 2 (NF2) is a genetic disorder characterized by the development of benign tumours, especially affecting the nervous system.
- It is autosomal dominant and affects approximately 1 in 40,000 individuals.
- NF2 is much less common than Neurofibromatosis Type 1 (NF1).
- There is often a family history of NF2, though some cases arise from de novo mutations.
🧬 Aetiology
- The NF2 gene is located on chromosome 22, encoding a tumour suppressor protein called Merlin (also known as Schwannomin).
- Merlin is involved in maintaining the structure of the cytoskeleton and preventing uncontrolled cell growth, particularly in nerve cells.
- Loss of function of the NF2 gene leads to the development of various tumours in the central and peripheral nervous systems.
🩺 Clinical Features
- Bilateral Vestibular Schwannomas (Acoustic Neuromas): These are the hallmark of NF2 and can lead to hearing loss, tinnitus, and balance issues due to involvement of the eighth cranial nerve.
- Juvenile posterior subcapsular lenticular opacity: A cataract that occurs at an early age, leading to potential blindness.
- Other brain and spinal cord tumours such as meningiomas, ependymomas, astrocytomas, and gliomas are frequently observed in NF2 patients.
- Spinal tumours like intramedullary gliomas and ependymomas occur with increased frequency.
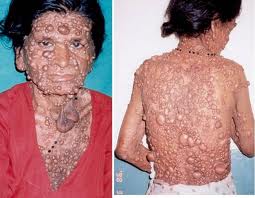
- Cutaneous features: Though less pronounced than in NF1, patients may develop cutaneous neurofibromas and subcutaneous nodules.
- Other clinical signs include plexiform neuromas and optic nerve gliomas, which may lead to vision loss.
Associations
- Pulmonary Fibrosis: A rare but recognized complication in NF2.
- Hypertrophic Cardiomyopathy: Cardiac involvement in some patients.
- Skeletal Abnormalities: Scoliosis and local gigantism of a limb may be seen.
- Secondary Hypertension: May occur due to Phaeochromocytoma or Renal artery stenosis.
- Orbital Haemangiomas: Benign vascular lesions affecting the orbit, potentially leading to visual impairment.
💊 Management
- Supportive Care: Given the chronic nature of the disease, management is focused on symptom control and addressing specific complications such as hearing loss, visual impairment, and tumour growth.
- Regular Monitoring: MRI is the preferred imaging modality for monitoring brain, spine, and peripheral nerve tumours.
- Auditory Brainstem Implants (ABI): These may be considered in cases of severe hearing loss due to bilateral vestibular schwannomas.
- Genetic Counseling: NF2 is inherited in an autosomal dominant pattern, so genetic counseling is important for affected families.
- Secondary Hypertension Management: Screen for Phaeochromocytoma and Renal artery stenosis if secondary hypertension is suspected. Treat appropriately with antihypertensives and possible surgical intervention for Phaeochromocytoma.
References
Cases - Neurofibromatosis Type 2 (NF2)
- Case 1 - Bilateral Vestibular Schwannomas 👂: A 23-year-old woman presents with progressive bilateral hearing loss and imbalance. Exam: bilateral sensorineural hearing loss, absent corneal reflexes. MRI: bilateral vestibular schwannomas. Diagnosis: NF2 (pathognomonic feature). Management: Regular MRI monitoring, hearing aids/cochlear implants, surgery or radiosurgery for tumour growth; genetic counselling.
- Case 2 - Spinal Cord Tumours 🧠: A 29-year-old man reports progressive leg weakness and numbness. Exam: spastic paraparesis, sensory level at T8. MRI spine: multiple intradural schwannomas and meningiomas. Family history: father had “brain tumours” in his 30s. Diagnosis: NF2 with multiple spinal tumours. Management: Neurosurgical referral for decompression; regular neuroimaging; physiotherapy and MDT rehab.
- Case 3 - Juvenile Cataracts 👓: A 16-year-old girl presents with painless, progressive visual blurring. Ophthalmology exam: posterior subcapsular cataracts. Further workup due to family history of NF2 reveals a unilateral vestibular schwannoma on MRI. Diagnosis: Early NF2 presenting with ocular involvement. Management: Cataract extraction; ongoing surveillance with MRI brain/spine; genetic testing and family screening.
Teaching Commentary 🧠
NF2 is a rare, autosomal dominant disorder due to NF2 gene mutation on chromosome 22, causing loss of tumour suppressor protein merlin. Key features: - Bilateral vestibular schwannomas (diagnostic hallmark) → progressive hearing loss, tinnitus, imbalance. - Other tumours: meningiomas, ependymomas, schwannomas elsewhere. - Ocular: early cataracts, retinal hamartomas. Dx: MRI brain/spine, genetic testing. Mx: surveillance + surgery/radiosurgery for tumours; hearing support; cataract surgery; genetic counselling. Prognosis: variable, but progressive neurological disability common by mid-adulthood.
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
