| Download the amazing global Makindo app: ✅ Means NICE/National Guidelines 2026 compliant Android | Apple | |
|---|---|
| MEDICAL DISCLAIMER: Educational use only. Not for diagnosis or management. See below for full disclaimer. |
Ehlers-Danlos syndromes
Related Subjects: |Autosomal Dominant |Autosomal Recessive |X Linked Recessive
🌟 Ehlers-Danlos Syndromes (EDS) are a group of inherited connective tissue disorders caused by defects in collagen synthesis and structure. Collagen is the scaffolding protein of skin, joints, vessels, and organs-so when it is faulty, the entire support system of the body is weakened. Common hallmarks include 🤸 joint hypermobility, 🧵 skin hyperextensibility, and 💥 tissue fragility, but the specific presentation varies across subtypes.
📖 About
- A heterogeneous collection of conditions, historically classified as EDS I–X, now recognized as 13 subtypes.
- Overall prevalence ~1 in 5,000 births 👶.
- Most forms are autosomal dominant, though some are autosomal recessive.
- EDS represents a spectrum: some mild with joint laxity, others life-threatening with vascular rupture.
🧬 Aetiology
- Mutations in genes encoding collagen or enzymes that process collagen (e.g., COL5A1, COL3A1, PLOD1).
- Defective collagen biosynthesis → abnormal fibrils → weak connective tissue.
- Faults in post-translational modification (e.g., hydroxylation, cross-linking) impair tensile strength.
- Take-home: study collagen pathways-EDS is essentially “molecular scaffolding gone wrong.”
Gorlin’s sign 👅
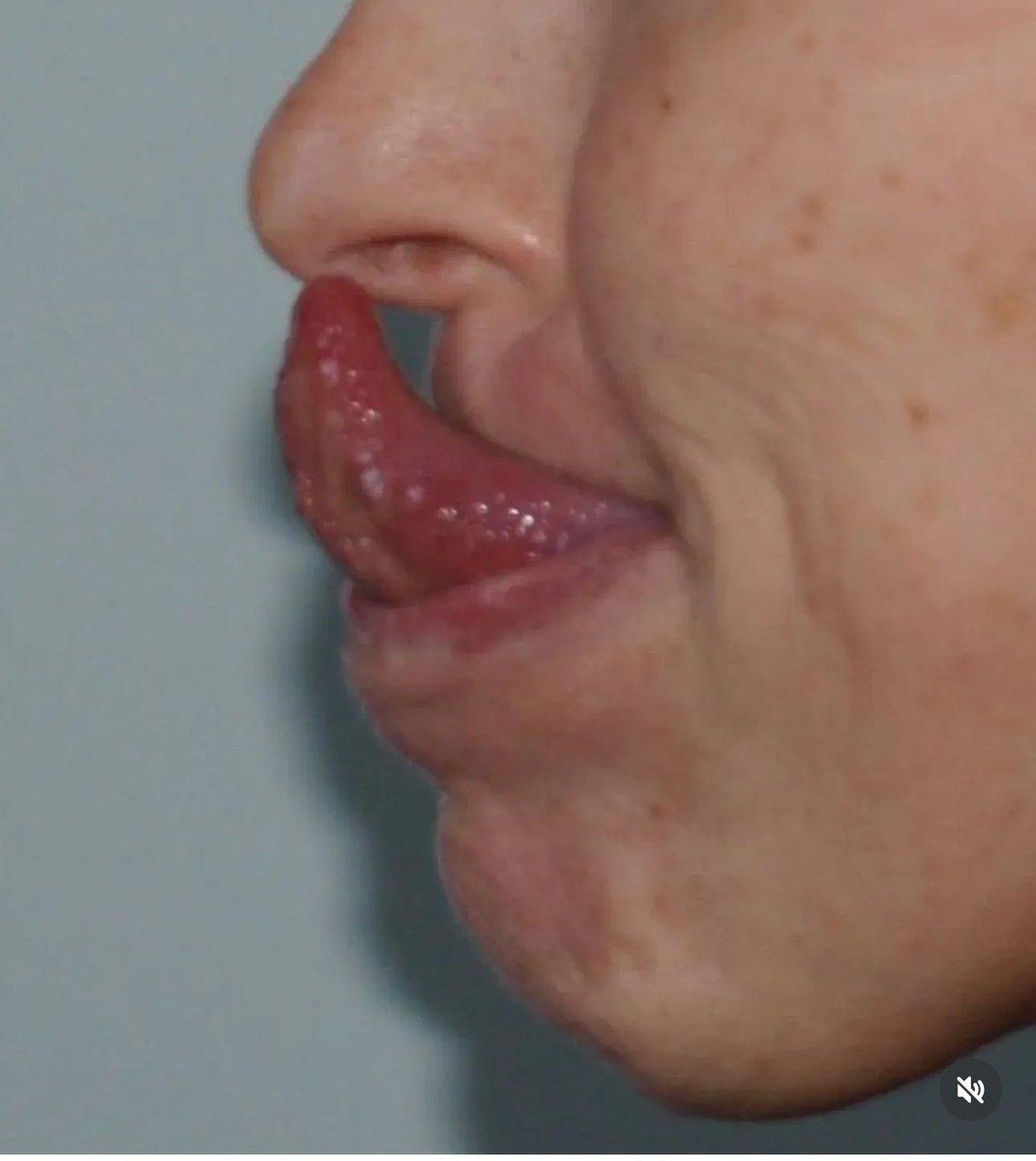
🔎 Types of Ehlers-Danlos Syndromes
There are 13 recognized subtypes; the most important exam-relevant ones include:
- Hypermobile EDS (hEDS) 🤸: Most common; marked joint hypermobility, chronic pain, soft/velvety skin. Genetics still not fully defined.
- Classical EDS (cEDS) 🧵: Soft, hyperelastic skin, widened atrophic scars, frequent bruising, joint laxity. Mutations in COL5A1/2.
- Vascular EDS (vEDS) 💔: Most dangerous; fragile arteries, risk of rupture, bowel and uterine rupture. Associated with COL3A1 mutation.
- Kyphoscoliotic EDS (kEDS) 🌀: Severe congenital scoliosis, hypotonia, ocular fragility. Caused by PLOD1 mutations (lysyl hydroxylase deficiency).
- Arthrochalasia EDS (aEDS) 🦴: Severe congenital hip dislocations, extreme joint hypermobility, fragile skin.
- Dermatosparaxis EDS (dEDS) 🩹: Extremely fragile, sagging skin; hernias. Caused by ADAMTS2 mutation.

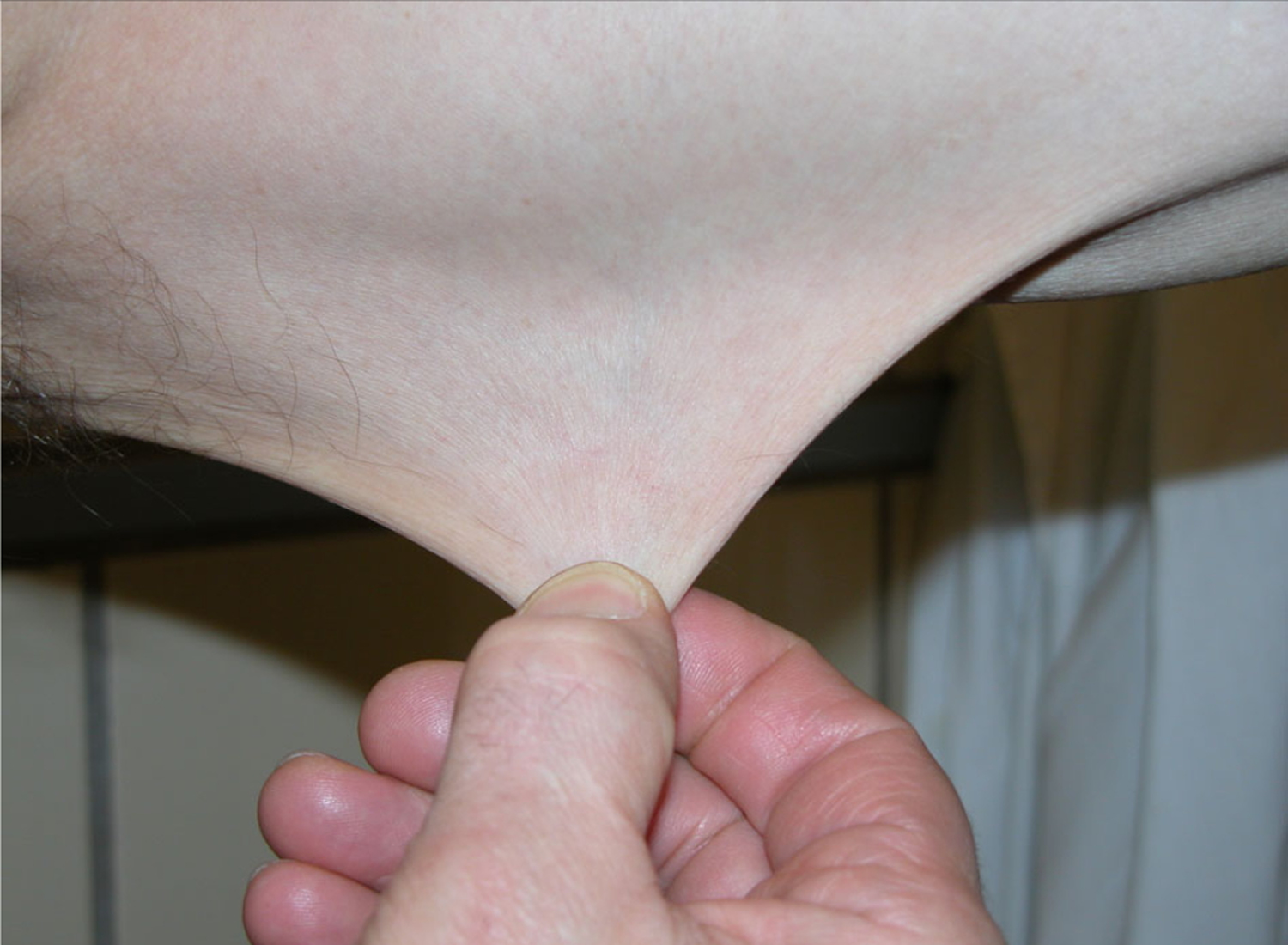
🩺 Clinical Features
- 🤸 Joint hypermobility: “party trick” joints but prone to sprains/dislocations.
- 🧵 Skin hyperextensibility: Soft, stretchy skin, sometimes with cigarette-paper scars.
- 💥 Tissue fragility: Easy bruising, poor wound healing, atrophic scars.
- 🩹 Musculoskeletal: Chronic pain, fatigue, frequent dislocations, scoliosis.
- 👁️ Ocular: Fragile sclerae → risk of globe rupture (esp. in kEDS).
- ❤️ Cardiovascular: Aortic dilatation, mitral valve prolapse, vascular rupture in vEDS.
- ⚠️ GI: Bowel rupture, hernias.
🧾 Differentials
- Familial Joint Hypermobility (benign, no tissue fragility)
- Marfan’s Syndrome (tall habitus, lens dislocation, fibrillin mutation)
- Larsen’s Syndrome (joint dislocations, craniofacial features)
🧪 Investigations
- Clinical criteria: Beighton score for hypermobility, skin/vascular signs.
- Family history: Key to inheritance pattern.
- Genetic testing: Confirms subtype (esp. vEDS via COL3A1).
- Imaging: Echocardiography for aortic root; MRI for scoliosis/joint pathology.
- Skin biopsy: Can show abnormal collagen fibrils (research/rarely clinical).
Beighton score (0–9) 🦴
The Beighton score is a quick bedside screen for generalised joint hypermobility. It scores 5 manoeuvres (4 are bilateral) to give a total out of 9 - it supports (but does not diagnose) hypermobility spectrum disorders / hEDS. Hypermobility reflects increased connective-tissue laxity (collagen/ECM mechanics), so pair the score with symptoms (pain, sprains, dislocations, dysautonomia features) and skin/family history.
- 1 point each side: Passive dorsiflexion of the 5th finger > 90° (R / L)
- 1 point each side: Thumb touches the forearm (R / L)
- 1 point each side: Elbow hyperextension > 10° (R / L)
- 1 point each side: Knee hyperextension > 10° (R / L)
- 1 point: Palms flat on the floor with knees straight (forward flexion)
- Common cut-offs: ≥ 5/9 adults, ≥ 6/9 children/adolescents, ≥ 4/9 if >50 years (thresholds vary by guideline/context).
- Practical tip: score what you see today (don’t “award for history”), but note pain, prior surgery, and guarding can reduce apparent hypermobility.
💊 Management
- Physiotherapy 🤸: Strengthen periarticular muscles; prevent dislocations.
- Pain management 💊: Paracetamol, NSAIDs, avoid long-term opioids; sometimes neuropathic pain agents.
- Protective strategies 🦾: Braces, taping, mobility aids, avoiding high-impact sports.
- Cardiac surveillance ❤️: Especially in vEDS (yearly echo, vascular imaging).
- Surgery 🩺: High risk due to fragile tissues-reserved for emergencies or severe complications.
- Genetic counseling 🧬: For patients and families.
📌 Clinical Pearls
- Not every hypermobile patient has EDS-distinguish from benign hypermobility.
- vEDS = ⚠️ think “vascular catastrophe” → young person with spontaneous arterial rupture, uterine rupture, or bowel perforation.
- EDS scars often look like “cigarette paper” 🚬-thin, papery, and stretched.
- Always screen for psychological burden-chronic pain & fatigue are disabling.
Categories
- About
- Acute Medicine
- Anaesthetics and Critical Care
- Anatomy
- Anatomy and Physiology
- Biochemistry
- Book
- Cardiology
- Collections
- CompSci
- Crib Sheets
- Critical care
- Dental
- Dermatology
- Differentials
- Drugs
- ENT
- Electrocardiogram
- Embryology
- Emergency Medicine
- Endocrinology
- Ethics
- Foundation Doctors
- GCSE
- Gastroenterology
- General Practice
- Genetics
- Geriatric Medicine
- Geriatrics
- Guidelines
- Haematology
- Hepatology
- Immunology
- Infectious Diseases
- Infographic
- Investigations
- Lists
- MRCP
- Mandatory Training
- Medical Students
- Microbiology
- Nephrology
- Neurology
- Neurosurgery
- Nutrition
- OSCE
- Obstetrics Gynaecology
- Oncology
- Ophthalmology
- Oral Medicine and Dentistry
- Orthopaedics
- Paediatrics
- Palliative
- Palliative Care
- Pathology
- Pharmacology
- Physiology
- Procedures
- Psychiatry
- Public Health
- Radiology
- Respiratory
- Resuscitation
- Revision Topics
- Rheumatology
- Statistics and Research
- Stroke
- Surgery
- Toxicology
- Trauma and Orthopaedics
- USMLE
- Urology
- Vascular Surgery
